ROPA Method, lesbian, bisexual and transgender motherhood
Reproductive medicine offers different alternatives for new family models, among them, the ROPA method that allows couples to share motherhood from the beginning. One as the genetic mother and the other as the gestational mother.
Reproductive medicine offers different alternatives for new family models, among them, the ROPA method which allows couples to share motherhood from the beginning. One as the genetic mother and the other as the gestational mother.
What is the ROPA method?
Sexual reproduction requires the interaction of two germ cells: a female and a male, inside female genitalia. When, for reasons of sexual identity or orientation, this process is not accepted, we resort to Assisted Reproduction Techniques because sexuality and the desire to procreate do not necessarily have to be linked to these biological conditions.
Nowadays we face family diversity. Situations and desires are so heterogeneous that specific responses are required for each situation, such as pregnancy between two women.
At Instituto Bernabeu, always sensitive to the specific needs of each patient, we adapt our medical and reproductive care to offer personalised treatments.
ROPA method requirements.
The requirements to be met by a couple undergoing ROPA treatment are:
- Be of legal age (over 18 years of age) at the start of treatment.
- Have full capacity to act voluntarily.
- Give the required written consent.
- Not suffer from any serious life-threatening illnesses for the mother or the unborn child.
In addition, there are legal requirements for the ROPA method, which are detailed below.
The legal situation of motherhood in Spain for lesbian couples.
According to current Spanish legislation in force, ‘Women may be users of the techniques regulated in this law regardless of their marital status and sexual orientation’. Thus, the right to motherhood is reinforced for all women and more importantly: not only for reasons of sterility.
Since 2007, Spanish Law allows the registration of double motherhood in the Civil Registry, so that children born from a ROPA treatment in Spain, between a married couple of women, will be children of two mothers for legal purposes, as long as both women are married. Furthermore, the recent Law 4/2023, of 28 February, for the real and effective equality of trans people and for the guarantee of the rights of LGTBI people, also contains in its final provisions (1st and 11th) in which heterosexual couples are equated with homosexual couples (married or not) for the purpose of facilitating the recognition of the double maternal filiation of their members.
If they are not married or are in a female domestic partnership at the time of undergoing IVF, but get married or enter into a domestic partnership before the child is born, they can also take advantage of the above legal provision and proceed in the same way.
In the event that pre-embryos from a ROPA treatment are frozen, it is not necessary to transfer them to the same woman of the couple who transferred them in the first treatment, unless there is a medical indication to do so, since, being married or in a common-law relationship, the pre-embryos belong to both members of the couple, and can be transferred to either of them in a subsequent cycle.
IVF ROPA or double motherhood treatment (receiving oocytes from the partner).
In addition to the conventional assisted reproduction techniques that lesbian couples have been choosing: artificial insemination, in vitro fertilisation (IVF), egg donation or embryo adoption, we offer them a new alternative of shared maternity: the reception of oocytes from their partner – the ROPA method.
At present, although it is a technique not provided for in the Law, it is possible to access the ROPA technique or reception of oocytes from a couple, which allows two women who are members of a married or common-law couple to participate in the treatment and the pregnancy. One provides the oocytes that are inseminated with sperm from an anonymous donor, and the other receives the embryos to become pregnant. There is a genetic mother and a gestational mother after both have given their consent. For this purpose, since 2007, the Spanish law allows the registration of double maternity in the Civil Registry as long as the couple is a homosexual marriage or a common-law couple, so that children born from a ROPA treatment will be children of two mothers for legal purposes.
How does the ROPA method work?
The ROPA method is nothing more than a conventional In Vitro Fertilisation (IVF) treatment carried out by qualified professionals in an assisted reproduction centre and adapted to the reproductive needs of lesbian women.
1. First of all, the study of both patients is required in order to individually design their treatment according to their medical needs.
2. Subsequently, the ovarian stimulation cycle is started in order to obtain a greater number of oocytes, and thus increase the probability of obtaining suitable embryos.
3. Simultaneously, your recipient partner undergoes endometrial preparation to facilitate embryo nesting.
4. Once the oocytes (eggs) have matured, the oocytes obtained in the laboratory are extracted and inseminated with donor sperm from our own sperm bank.
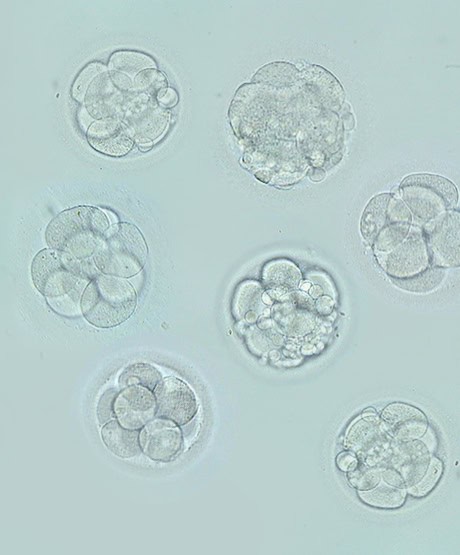
5. From this moment on, the embryos will begin to develop and will be transferred between the 5th and 6th day of development. This way we manage to carry out the embryo transfer at the blastocyst stage in order to optimise the chances of becoming pregnant, thus achieving high success rates.
6. The following months of gestation will develop like any other pregnancy, allowing both of you to share the miracle of life.
Furthermore, epigenetics has shown how factors in the environment and lifestyle of the mother responsible for the gestation will mark and determine the expression of the future baby’s genes, and therefore also participate genetically in its development. Any assisted reproduction treatment (in vitro fertilisation, embryo adoption or fertilisation using the ROPA method) has an emotional impact. In order to help our patients to cope with this, Instituto Bernabeu offers them, if they wish and at no extra cost, an individualised psychological session to prepare them to face the possible emotions associated with each phase of the reproductive process.
Our sperm donors for the ROPA method: the most rigorous selection
The choice of the most suitable donor involves the most comprehensive medical, physical and psychological analyses in order to offer you absolute security.
The process for choosing the most suitable sperm donor is very rigorous. It responds to the great responsibility we assume in view of the trust our patients have placed in us. That is why in sperm donation we carry out tests beyond those required by law. Due to the exhaustive nature of these tests, only a very select number of applicants are finally suitable for inclusion in our donor sperm bank. Only 9% of the candidates pass the strict psychological, genetic and medical tests that are compulsory.
Current technological advances allow us to develop additional analyses that offer greater security. To the controls that we carry out as a protocol in the donation process, we add the study of sexually transmitted diseases, genetic analysis of the 600 or 3,000 most serious diseases that can be transmitted to offspring and, among others, blood analysis by PCR, which gives the opportunity for a second validation of serologies at the time of extraction, since the diagnosis is immediate. And all this at no additional cost to the treatment.