IVF DOUBLE GAMETE DONATION
Double gamete donation is the most successful type of reproductive technique available. It entails transferring developed embryos generated after fertilisation of donated oocytes with donated sperm
What is in vitro fertilisation with double donation?
The procedure entails performing IVF treatment using gametes obtained through an oocyte donor sperm donor. The donated oocyte and sperm are used to generate an embryo that is implanted in the recipient patient during blastocyst stage. Law requires that the identity of both the donors and the recipients be absolutely confidential.
Double donation is the assisted reproduction technique that gives the best results. The reasons for this include exhaustive donor selection processes performed by Instituto Bernabeu during which we rule out the transmission of over 600-3000 genetic disorders. Donors also undergo a psychological, general health and reproduction (fertility and genetics) assessment. In addition to the fact that donors are young, this significantly reduces the risk of pregnancy loss, malformations and genetic abnormalities.
Double donation at Instituto Bernabeu
Instituto Bernabeu has been a leading entity in gamete donation since 1992 and this is mainly as a result of the following commitments:


Blastocists
All double donation transfers are performed during blastocyst stage. The chances of implanting during this phase of embryo development are higher than when transfer is performed earlier on. Should we be unsuccessful, we commit to giving patients an additional course of treatment at no additional cost.
In-house storage bank
We have our own donor programme. Our semen bank has been running since 1985 and it was one of the first semen banks in Europe. This means we are able to control traceability at all times and ensure rigorous donation processes as well as increased agility because there are no waiting lists.

Similarities in phenotype
We take donors’ physical features very much into account with the aim of ensuring that they are as similar as possible to the recipient mother’s features. The main features taken into account are face shape, skin tone, hair colour and type, eye colour, height, weight, blood group, Rh and so on.

Rigorous selection from a medical, psychological and genetic perspective
In addition to compliance with the provisions of Spanish laws on assisted reproduction treatment involving donors, Instituto Bernabeu applies the strictest of controls in order to be able to give our patients the assurance that, before being accepted onto our donor programme, donors have passed the strictest of medical, genetic, psychological and socio-cultural controls.

Age is a factor
The average age of our oocyte donors is 24 and they are never older than 33. Semen donors are never over 35 years of age.
-Medical check-up and analysis of the donor’s medical background and the medical background of his/her family members.
-Gynaecological analysis
-Psychological analysis
-Genetic Analysis
Only 22% of potential egg donors and only 9% of sperm donor candidates pass these strict tests. Some of the main reasons for exclusion include sperm quality (mobility, motility and sperm count).*
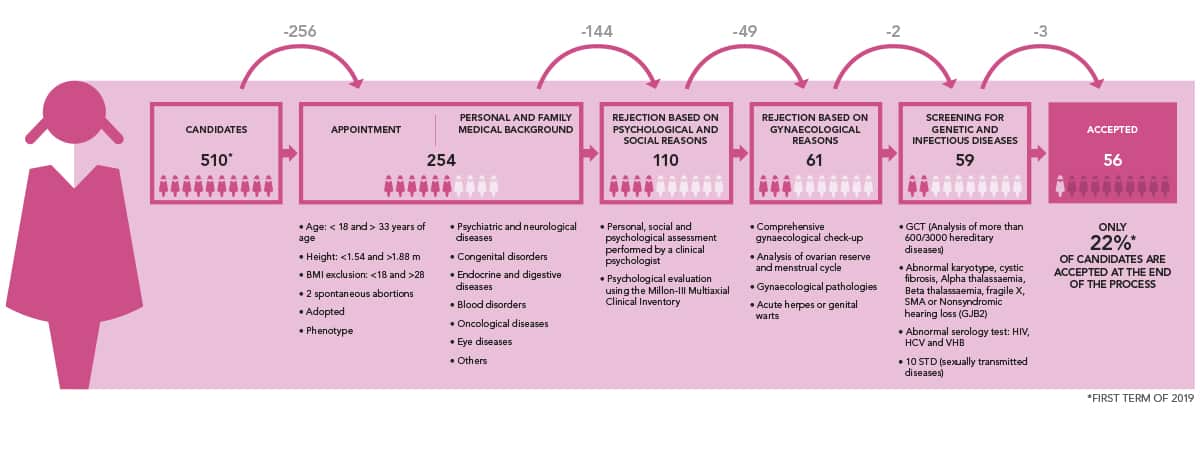
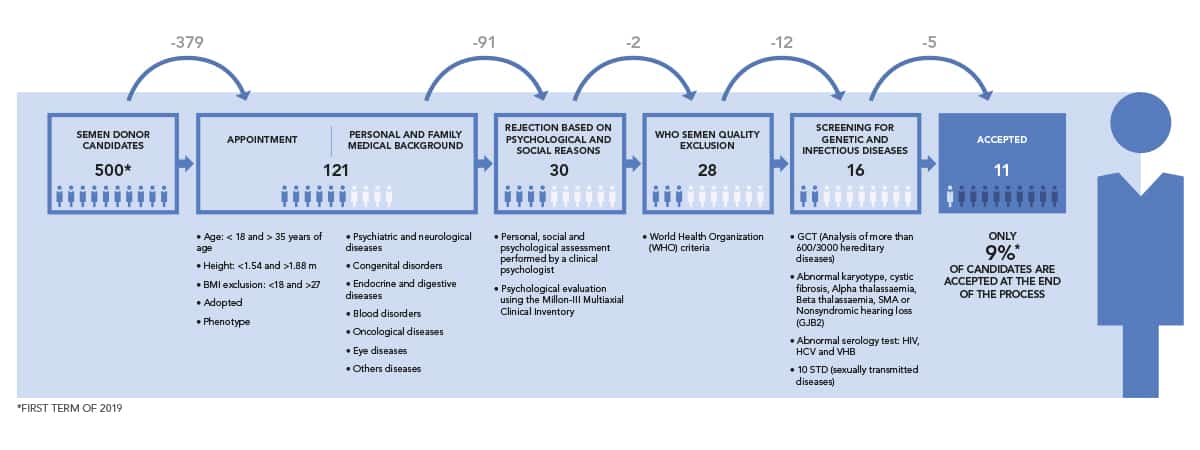
(*) statistics based on 2019 first term over 510 female candidates and 500male candidates.
Genetic Compatibility Test (GCT) performed on both donors
We look after the health of the future baby, which is why we carry out the most complete recessive disease test (more than 600 or 3000 hereditary diseases, depending on the modality) at no added cost, to each of the donors( also known as carrier genetic test (CGT)®, Carriermap®, CarrierDNAinsight® o Recombine®.


Duration of double donation treatment
Gamete double donation treatment takes between approximately 6 and 8 weeks to complete. This is the time that we need to select the most appropriate donors and prepare the ovarian stimulation cycle. Following oocyte retrieval, we perform in vitro fertilisation using the donor sperm. When the embryos reach blastocyst stage, they are transferred to the recipient patient and unused embryos are frozen by means of vitrification. We need to wait between 8 and 10 days before performing a pregnancy test.
Epigenetics and gamete donation
Epigenetics is a science that studies how certain environmental factors and the mother’s lifestyle (for example, nutrition, smoking, drinking and exercise) can affect the expressions in certain genes. The gestating mother also has an impact on the future child’s development and can influence certain genetic expressions.
IVF DOUBLE DONATION TREATMENT PHASES

1 day

FIRST VISIT
Starting a treatment that uses donated egg cells is a very important decision that must be made with all the necessary information. For this reason, the doctor in charge of your case will provide you with detailed information about possible alternatives and the most relevant aspects of the treatment.
It is crucial that you are provided with detailed information about those aspects having to do with the donor, both as regards legislation and the selection procedures that are required to accept candidates as donors. Fortunately, legislation in Spain is clear, and it offers a legal security framework that allows treatments to be carried out in a simple way.
You will also receive information on the procedures followed to select the best donor for you based on your physical and clinical traits.
On this visit, and once you have agreed to take the treatment and selected a time frame to complete it, you will receive information on the necessary steps to get started. The arrangements to receive the embryos are much simpler than the ones for in vitro fertilization (IVF): they do not include daily injections and the number of visits for ultrasound control is limited. You could receive an approximate start date for the treatment at this moment.
At the end of your appointment with the gynecologist you should meet with your Comprehensive Care Provider to complete all the medical and legal requirements (i.e. to sign consents) and receive prescriptions for the necessary drugs as well as accurate and detailed instructions to use them.
Furthermore, at no additional cost and on voluntary basis, you can have a face-to-face meeting with a clinic psychologist from our egg donation department who will explain the assignment and selection process of the most suitable donor and will answer any related queries you may have.

DESIGNING THE TREATMENT AND SYNCHRONIZING
From the moment when patients are advised to undergo double donation and accept this treatment option, a process that entails coordination between all the departments at IB is initiated. The aim is to give patients the very best chances of success based on the foundations of excellent care.

15/35 days
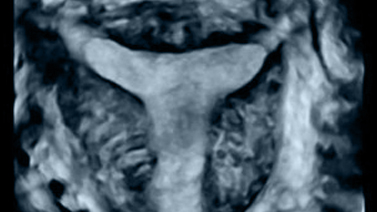
Preparing the endometrial cavity to receive the embryo
The endometrium is the uterus “layer” where the embryo attaches and subsequently implants so that pregnancy can take place.
The endometrium is the uterus “layer” where the embryo attaches and subsequently implants so that pregnancy can take place.
This “layer” should be prepared and synchronized with the embryo. For this reason, drugs need to be administered to send the right signs to the uterus so that its “receptivity” is optimal.
Fortunately, preparation is extremely simple: injections, tests and frequent appointments are not necessary at this stage.
The drugs needed for the treatment are administered orally or transcutaneously (i.e. patches) and have a high tolerance level, as the hormone levels that are sought are very similar to those in women during their natural cycle.
After oocytes have been retrieved from the donor, administration of progesterone begins, normally via vagina (vaginal tablets). The beginning of progesterone administration is extremely important as it is when the sign for the endometrium to be receptive at the moment of transfer is “sent”. In other words, is what creates the correct synchronization between the embryo and the uterus.
You will receive accurate and detailed written instructions about each and every step for preparation. Even so, the whole of our team is at your disposal, so please do not hesitate to let us know if you have any questions or concerns.

Selecting the most appropriate donors
We are aware of the huge responsibility our team undertakes and, in these cases, we begin by performing a strict selection of the most appropriate sperm and egg donors in order to guarantee quality and the very best possible results for our patients.
After passing strict psychological, gynaecological and genetic tests with a negative result for the main hereditary diseases, candidates are accepted as egg donors. In addition to the genetic and medical tests, sperm donors must also pass the strict Instituto Bernabeu sperm count, sperm mobility, sperm motility and sperm freezing tests. These include, for example, a minimum of 80 million in the sperm count (the World Health Organization indicates that 15 million is a normal result).
Donors take a genetic carrier test (GCT) for the 600 most common genetic disorders and the ones that have the greatest impact on a person’s health.
Previously, the recipient couple has informed us about their blood type and their main physical characteristics (weight, height, skin tone, hair and eyes colour, and so on) and will provide different photographs to make the search easier. According to the Spanish legislation, under no circumstances, the donors’ nor the parents’ identity will be disclosed. Yet, the results of the medical and gynaecological tests and the donors’ age may be disclosed in case it is needed in the future. In addition, the donors’ genetic material (DNA) will be kept in custody for a period of 20 years in case it becomes necessary to carry out advanced comparative genetic study of the future newborn.
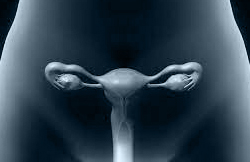
STIMULATING THE DONOR’S OVARIES
Stimulation of the donor’s ovaries begins at the same time as the therapy to develop the recipient mother’s endometrium. Stimulation is key to future success. It is important to produce the highest possible amount of oocytes, but it is even more important to ensure their quality.

1 day

RETRIEVING THE DONOR’S EGGS
At Instituto Bernabeu, we guarantee our egg donation receptor patients a minimum of 8 mature oocytes and an average of 11.
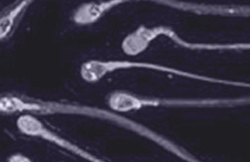
SPERM CAPACITATION
We simultaneously proceed to defrost the donor sperm. The sample is capacitated in the laboratory in order to optimise its ability to fertilise.
IN VITRO FERTILISATION
Fertilisation is carried out in the human embryology laboratory by joining the oocyte and the sperm, either by classic IVF -more natural- or using the ICSI technique, which consists of selecting a suitable spermatozoon and place it directly inside the oocyte through a fine needle, which in cases of male pathology makes fertilisation easier.
The result of fertilization (day 1 of the embryos’ life) can be seen within approximately 18 hours. At this point the amount of naturally fertilized oocytes, which is the same as the number of embryos, can be determined.
STARTING TO TAKE PROGESTERONE
Just like it happens in a woman’s natural cycle, progesterone must be included in the recipient mother’s medication at the time of fertilization. This drug is extremely important, as the fetus will need it during the first months of pregnancy, until s/he produces enough placenta.

3/5 days

CULTURING THE EMBRYOS
Fertilisation is followed by development in a culture medium that provides everything that is needed for growth. The embryos are assessed during development.
Growth is periodically assessed because not all human embryos reach blastocyst stage.
It is important to keep in mind that not all of them will fertilise and become viable embryos. There will be good and poor quality embryos and others that will simply block.
In our donation cycles, 75% of embryos reach blastocyst stage and 100% of transfers are performed on day 5 or 6.

1 day
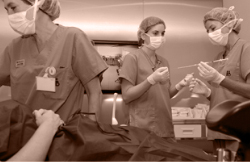
TRANSFERRING THE EMBRYOS
Once the blastocyst stage has been reached, embryo transfer takes place. It is an essential stage during treatment. It entails placing the embryo in the mother’s uterus.
The procedure is performed using an abdominal ultrasound scan. The culture medium containing the embryo is positioned inside the uterus. It is a quick and painless procedure.
Embryos that have not been transferred and wish to be preserved, after vitrification, proceed to storage. After identification, they are deposited in an exclusive location in the cryogenic tanks of our laboratories. For complete security, this location is not shared with other samples, nor with other patients, to protect them from potential cross-infection or inaccuracies.
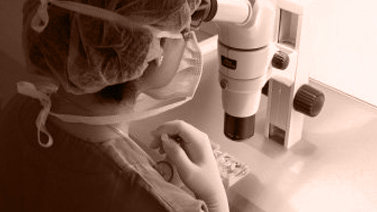
FREEZING EMBRYOS
It is common for several embryos to reach the blastocyst stage following dual donation treatment. Therefore, the embryos that are not initially transferred are frozen by means of vitrification.

10/12 days

TESTING FOR POSITIVE PREGNANCY
13/14 days after the progesterone medication began, a blood sample is taken from the patient in order to determine if she is pregnant or not. It consists of detecting beta-hCG levels in blood since this hormone is produced by the embryo and passed on to the mother. It is the first measurable sign sent by the embryo.
If the patient is not pregnant, the medical team involved in the course of treatment assesses the causes and decides what steps need to be taken. The patient is given an appointment in order to be able to tell her about the team’s evaluation of the situation.

15 days later
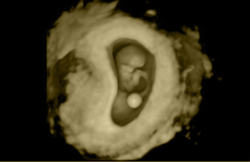
PREGNANCY ULTRASOUND
If the result of the pregnancy test is positive, the patient has an ultrasound scan around two weeks later. Performing this scan any earlier would lead to confusion and doubts since the results are generally not conclusive at this stage.
THERE WILL ALWAYS BE EMBRYO TRANSFER. When patients undergo double donation, Instituto Bernabeu guarantees transfer during blastocyst stage.
IVF double gamete donation treatment success |
||
| Accumulative positive pregnancy rate over 3 cycles | 94,1% | |
| Positive pregnancy rate (including frozen embryo transfers) | 92,6%* | |
| Fresh embryo donation | 94% (We synchronise procedures to ensure fresh egg donation, except when the contrary is expressly requested by the recipient) |
|
Cycles of egg donation with embryo freezing (an average of 2.3 blastocysts per cycle) |
89,7% and an average of 3.8 blastocysts | |
| Transfers on day 5-6 (blastocyst) | 100% | |
| Embryos reaching blastocyst stage | 76,4% | |
| All our egg donors are thoroughly screened | Maximum rigor: – Psychological, physical, gynaecological and fertility evaluations. – Complete analyses: blood tests, serology (HIV, hepatitis B and C, syphilis, etc.), karyotype, cytomegalovirus, Fragile X syndrome, alpha thalassaemia, beta thalassaemia and muscular spinal atrophy and nonsyndromic hearing loss (GJB2), electrocardiogram, screening for 10 sexually transmitted diseases. |
|
| Analysis of 600/3000 autosomal recessive disorders (gct: genetical analysis in disorder carriers) | Carried out on all our donors at no cost for the patient. This allows us to identify the presence of mutation in 555 genes causing more than 600 diseases or 2306 genes that causes more than 3000 hereditary diseases. |
|
| State-of-the-art technology associated with the treatment at no cost (if medicallyadvised) |
|
|
| Viable pregnancy 100% guaranteed | Optional (subject to medical criteria). Read More |
|
