Egg donation, IVF treatment with donated eggs
The most reliable assisted reproduction technique involves anonymous donated eggs which, following fertilization, are transferred to the recipient patient to achieve pregnancy
What is egg donation?
Egg donation is currently one of the most effective assisted reproduction treatment available as it allows a woman who is unable to have children with her own eggs to experience pregnancy. In vitro fertilisation treatment (IVF) is performed using anonymous donor eggs which are fertilized using the partner’s sperm. The generated embryos are then transferred to the recipient mother.

1 day

Starting a treatment using donated eggs is a very important decision that must be made with all the necessary information. For this reason, the doctor in charge of your case will provide you with detailed information about possible alternatives and the most the treatment’s relevant aspects.
It is very important you are provided with detailed information about those aspects regarding the donor, both as regards legislation and the required selection procedures to accept candidates as donors. Fortunately, legislation in Spain is clear, and it offers a legal security framework allowing treatments to be carried out in a simple way.
You will also receive information on the procedures followed to select the best donor for you based on your physical and clinical traits.
On this visit, and once you have agreed to undergo treatment and selected a time frame to complete it, you will receive information on the necessary steps to get started. The arrangements to receive the embryos are much simpler than the ones for in vitro fertilization (IVF): they do not include daily injections and the number of visits for ultrasound control is limited. You could receive an approximate start date for treatment at this moment.
Once the appointment with the gynaecologist has finished, you should meet with your Patient Care Assistant to complete all medical and legal requirements (i.e. to sign consents) and receive prescriptions for the necessary drugs as well as accurate and detailed instructions to use them.
In addition, at no additional cost and on voluntary basis, you can have a face-to-face meeting with a clinical psychologist from our egg donation department who will explain the assign and selection process of the most suitable egg donor and will answer any related queries you may have.

From the very first moment you are indicated for egg donation treatment and decide to undergo this treatment, it begins a process where all the different departments in Instituto Bernabeu are coordinated to offer you the best possible chances of success with the best personal care.

15/35 days
The endometrium is the uterus “layer” where the embryo attaches and subsequently implants so that pregnancy takes place.
This “layer” should be prepared and synchronized with the embryo. For this reason, drugs need to be administered to send the right signs to the uterus so that its “receptivity” is optimal.
Fortunately, preparation is extremely simple: injections, tests and frequent appointments are not necessary at this stage.
The drugs needed for treatment are orally or transcutaneous (i.e. patches) administered and have a high tolerance level, as the hormone levels sought are very similar to those in women during their natural cycle.
After oocytes have been retrieved from the donor, administration of progesterone begins for the patient, normally vaginally (vaginal tablets). The beginning of the progesterone administration is extremely important, since it is when the sign for the endometrium to be receptive at the moment of transference is “sent”. In other words, it is what creates the correct synchronization between the embryo and the uterus.
You will receive accurate and detailed written instructions about each and every step for preparation. Even so, the whole of our team is at your disposal, so please do not hesitate to let us know if you have any questions or concerns.

Aware of the great responsibility your trust placed in our team entails, we begin a strict selection of the egg donor to guarantee the highest quality and best results to our patients.
Having successfully passed very strict analysis: psychological evaluation and medical, gynaecological and genetic tests, and negative result for the main diseases that could be transmitted; the candidate is accepted in the egg donor’s programme.
We carry out on all our donors, and at no extra cost, the study of more than 600 hereditary diseases and since 2020, the recessive diseases exome, allowing us to analyse mutations in 2306 genes causing more than 3000 diseases. As of today, is the most complete genetic screening performed on oocytes and sperm donors. If both parents are carriers of a variant mutation in the same gene, the disease will manifest itself. Therefore, these studies are only valid if they are compared with the other parent’s DNA. The test also allows us to detect X-linked diseases, ruling out donor candidates who may be carriers.
Previously, the recipient patient has informed us about her blood type and her general physical characteristics (weight, height, skin tone and eyes and hair colour and so on) and will provide different photographs to make the search easier. According to the Spanish legislation, under no circumstances, the donors’ or parents’ identity will be disclosed, but we will provide the patients with a report of the medical and genetic studies carried out, as well as the age in case it might me necessary in the future. In addition, the donors’ genetic material (DNA) will be kept in custody for a period of 20 years in case patients need additional genetic studies.
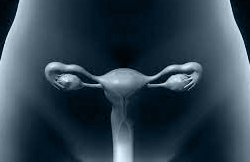
Stimulation of the donor’s ovaries begins at the same time as the therapy to develop the recipient mother’s endometrium. Stimulation is key to future success. It is important to produce the highest possible amount of oocytes, but it is even more important to ensure their quality.

1 day
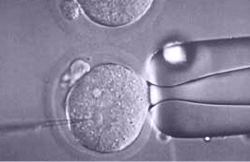
When the right time has come, the donor is put under sedation in the operating room and her eggs are retrieved.
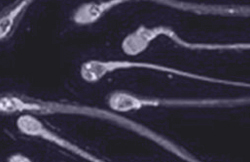
Simultaneously, the male provides a sperm sample. The sample is capacitated in the laboratory to increase its power to fertilize.

Fertilization is initiated in the Human Embryology Laboratory by joining an oocyte with the male’s sperm, either through the usual IVF procedure (more natural) or the ICSI procedure, whereby a single suitable sperm is injected into the oocyte through a thin needle. This procedure facilitates fertilization in cases of male pathology.
The result of fertilization (day 1 of the embryos’ life) can be seen within approximately 18 hours. At this point the amount of naturally fertilized oocytes, which is the same as the number of embryos, can be determined.
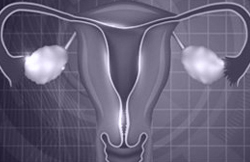
Just like it happens in a woman’s natural cycle, progesterone must be included in the recipient mother’s medication at the time of fertilization. This drug is extremely important, as the fetus will need it during the first months of pregnancy, until s/he produces enough placenta.

3/5 days

Fertilisation is followed by development in a culture medium that provides everything that is needed for growth. The embryos are assessed during development.
Growth is periodically assessed because not all human embryos reach blastocyst stage.
It is important to keep in mind that not all of them will fertilise and become viable embryos. There will be good and poor quality embryos and others that will simply block.
In our donation cycles, 75% of embryos reach blastocyst stage and 100% of transfers are performed on day 5 or 6.

1 day
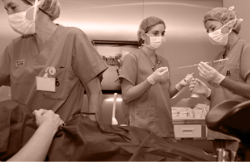
Once the blastocyst stage has been reached, the embryo transfer takes place. This is an essential step in treatment. It entails placing the embryo in the mother’s uterus.
The procedure is performed using an abdominal ultrasound scan. The culture medium containing the embryo is placed inside the uterus. This is a quick and painless procedure.
The transfer is carried out under respectful conditions that take into account the embryo’s sensitivity.
Embryos that have not been transferred and are to be preserved, after its vitrification and identification, are stored in an exclusive location in our laboratory’s cryogenic tanks. To secure safety, this location is not shared with other samples nor with other patients in order to protect them from potential cross-infections or inaccuracies.

10/12 days later

13/14 days after the progesterone medication began, a blood sample is taken from the patient in order to determine whether she is pregnant or not. It consists of detecting beta-hCG levels in blood as this hormone is produced by the embryo and passed on to the mother. This is the first measurable sign sent by the embryo.
If pregnancy is not achieved, the treatment’s medical team will assess the causes and will decide what further steps need to be taken. The patient is given a new appointment where she will be explained the team’s evaluation of the situation.

15 days later
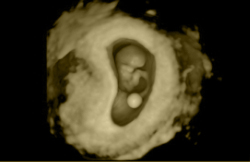
If the result of the pregnancy test is positive, the patient has an ultrasound scan around two weeks later. Performing this scan any earlier would lead to confusion and doubts since the results are generally not conclusive at this stage.
The most comprehensive analysis of hereditary disorders
We perform the most comprehensive test for the main hereditary disorders (over 600 or 3000 recessive diseases, depending on the test chosen). By doing so, we are safeguarding the health of your future child (genetic compatibility analysis or GCT). The test is performed on all donors at no additional cost. The GCT test is also known as Carrier genetic test (CGT)® Carriermap®, CarrierDNAinsight® and Recombine®.
Advantages of donating eggs
- It is the reproductive medicine technique with best results.
- It does not involve ovarian hormonal stimulation or daily injections for the recipient patient.
- It does not require anaesthesia or sedation.
- It has the lowest miscarriage rates caused by chromosomal disorders linked to patient’s age.
- Undergoing egg donation at Instituto Bernabeu also offers the patient peace of mind that each step of the treatment will be carried out flawlessly.
Why opt for anonymous egg donation?
Often and for many reasons (e.g., age, hereditary diseases, past surgical operations, and so forth), ovaries lose their ability to produce healthy egg cells. Oocytes are vital for conception. This makes anonymous egg donation necessary, as part of In vitro Fertilisation treatments.
In addition, egg donation legal aspects in Spain must be taken into account: anonymity and confidentiality.
Egg donation at Instituto Bernabeu
Instituto Bernabeu is a leading egg donation centre in Europe counting with one of the first programmes in Spain. Because of our experience of more than 20 years, the large number of egg cell donations in our repository and the social and cultural status of our donors, we can guarantee that:
- We will conduct rigorous medical and genetic screenings of donor candidates.
- We will select the most compatible donor from a medical perspective.
- At Instituto Bernabeu we guarantee that we will obtain at least 2 good quality blastocysts, which maximises the chances of success in the embryo transfer and improves the results of the treatment.
- We will perform a thorough selection of physical characteristics that are similar to the receptor’s.

TECHNOLOGY AND SPECIFIC TREATMENT UNITS
Our own cutting-edge technology and specialised professional for every therapeutic need:
Duration of egg donation treatment
Egg donation treatment usually lasts between one and a half and two months. Once the oocytes are collected, in vitro fertilization (IVF) is performed. After the transfer, it will take about 10 days to verify the pregnancy and five days after the positive result, the first pregnancy ultrasound is performed.
SUCCESS RATE STATISTICS FOR OOCYTE DONATION AT INSTITUTO BERNABEU 2024
Patient age | Success rate |
|
Positive pregnancy test with 1 fresh transfer | 64,6% |
|
Cumulative positive pregnancy test* (1 fresh transfer plus 2 cryotransfers, with no PGD and elective vitrification) | 91% |
|
| Clinical pregnancy with 1 fresh transfer | 52,2% |
|
Embryo quality | Success rate |
|
Cycles during which embryos are frozen (an average of 3-4 blastocysts) | 92,6% |
|
| Transfer performed during blastocyst stage (day 5) | 100% |
|
* Transfer of 1 fresh cycle plus 1 frozen cycle with no DGP/PGT and elective vitrification.
Our results are held on the register at the Spanish Fertility Society (SEF) and have been audited by external companies Applus® and Instituto Fidelitas.
Therapeutic needs and programs
All our egg donors are thoroughly screened
Maximum rigor:
Psychological, physical, gynaecological and fertility evaluations.
Complete analyses: blood tests, serology (HIV, hepatitis B and C, syphilis, etc.), karyotype, cytomegalovirus, Fragile X syndrome, alpha thalassaemia, beta thalassaemia and muscular spinal atrophy and nonsyndromic hearing loss (GJB2), electrocardiogram, screening for 10 sexually transmitted diseases.
Analysis of 600/3000 autosomal recessive disorders (gct: genetical analysis in disorder carriers)
Carried out on all our egg donors at no cost to the patient. This allows us to identify the presence of up to 555 genetic mutations that cause more than 600 diseases, or 2306 genes that cause over 3000 disorders.
Read More
There is also the possibility of contrasting the GCT with the future father to rule out that any future child would suffer from any of them.

State-of-the-art technology associated with treatment with no extra cost (if medically advised)
- ICSI (Intracytoplasmic sperm injection)
- Long-term culture to blastocyst
- MACS sperm selection
Viable pregnancy 100% guaranteed
Optional (subject to medical criteria). Read More

Selection the most suitable egg donor
At Instituto Bernabeu, we perform rigorous and comprehensive screenings of donor candidates, including psychological, clinical and genetic evaluations, in order to maximize the suitability and safety of the procedure:
- A psychological evaluation performed by a clinical psychologist. This evaluation includes a personal interview and completing our Million-III Inventory Questionnaire to evaluate the candidate’s personality.
- An evaluation of the candidate’s personal and family history performed by a gynecologist specialized in fertility, and a physical and gynecological examination that shows the candidate’s good state of health and excludes the possibility of a gynecologic pathology.
- Chromosomal and genetic studies to rule out the possible presence of hereditary diseases: Karyotype (including chromosomal polymorphisms associated with an increased risk of miscarriage), screening for Fragile X Syndrome, Thalassemia, Spinal Muscular Dytrophy (SMD). In addition, the DNA extracted for genetic testing is stored in a biobank for future testing.
- Screening of the 10 most common sexually transmitted diseases (chlamydia, gonorrhoea, herpes I and II, trichomonas, Treponema, Mycoplasma hominis and genitalium, ureaplasma, haemophilus).
- TCG also called “genetic matching”.Is the carriers genetic study in which we prevent and avoid the transmission of more than 600 or 3000 hereditary diseases.
Find out more about egg donor selection
Donor DNA Repository
Thanks to the donor DNA cryobank driven forward by Instituto Bernabeu since its pioneering launch in 2010, patients who need to make use of donated gametes for their fertility treatment can, at any time, make a request for a genetics study with a view to preventing and adequately treating possible diseases which might affect their children in the future (further to egg donor consent). No extra costs.
Epigenetics and egg donation
Epigenetics is a science based on studying how certain environmental factors and as well as lifestyle habits such as eating, smoking, drinking and exercising in the mother can have an impact on the expressions in certain genes. Evidently, the mother’s habits cannot have an impact on the embryo’s genetics but they do influence epigenetic markers. As such, the mother carrying the child also has an impact on the future child’s development and shapes certain genetic expressions. She is not merely a receptacle.
Egg donation legal aspects
It is worth pointing out the main aspects of Law 14/2006 on assisted reproduction techniques with regards to egg donation. They are explained below:
- Egg donation must be altruist and unpaid because one of the fundamental principles of Spanish healthcare legislation is that the human body and its cells cannot be commercialised.
- It is also a free and formal contract between the donor and the clinic that has the authorisation to perform the technique. As such, donor selection is the responsibility of the medical team at the clinic.
- The essential characteristic is anonymous donation and personal data and donor identity confidentiality guaranteed, both on behalf of the gamete bank and on behalf of the reproduction clinic.
- Only in exceptional circumstances when the life or health of the child is in danger can donor identity be revealed and only when revealing that information is absolutely essential.
Access additional information in IB FORUM