Urology and andrology
Learn about the most important aspects of the urinary system and the male genital system, the sexual and reproductive function of men and discover aspects of interest around the medical area that takes care of the reproductive and sexual health of men.

Erectile Dysfunction and Pregnancy, is it possible to have children?
Erectile dysfunction or commonly called ‘male sexual impotence’ is the inability to obtain or maintain an erection adequate for satisfactory sexual intercourse. Could it be considered a cause of infertility? The answer is yes, but […]

Become a father after the age of 40 – 50. Does it have any risks?
Many studies has been made on how older maternal age is related to a lower probability of achieving pregnancy. Higher miscarriages frequency and higher risk of certain chromosomal abnormalities in the foetus. But little attention […]

Prostate; How does prostatitis affect male fertility?
What is prostatitis? Bacterial prostatitis is a clinical condition caused by a bacterial infection of the prostate that produces urinary symptoms and affects male fertility. What are the prostatitis causes? The causative germs are detected […]

Testicular tissue freezing in patients with cancer
Testicular tissue freezing is the extraction and subsequent cryopreservation of this tissue to try to preserve the fertility of a patient who is going to undergo gonadotoxic treatment. One of the medical cancer treatments’ side […]

Anejaculation and fertility: What is it? Is there any treatment? Can I be a father?
Ejaculation disorders are one of the most common sexual disorders in the male population. These are common in urology consultations and a possible cause of infertility. What is anejaculation? Anejaculation is defined as a type […]
Seminal culture: sperm culture
Infertility affects about 15 % of couples seeking pregnancy. Approximately 50 % of these cases are attributable to the male couple. One of the potential causes traditionally described in the literature has been the presence […]

Testicle diseases and how they affect the male fertility
Infertility is described by the World Health Organization (WHO) as “a disease of the reproductive system defined by the inability to achieve a clinical pregnancy after 12 months or more of regular unprotected sex.” Therefore, […]
What is the spermatogenesis about?
Spermatogenesis is the process of the sperm formation, which are male gametes. It takes place in the testicular seminiferous tubules with an approximate duration of 62 to 75 days in the human species. Sperm formation […]
What is hypospermia? How can it be detected? How does it affect my fertility?
The World Health Organization (WHO) indicates that a man has hypospermia when the semen sample he produces when he ejaculates is below 1.5 mL. A semen analysis needs to be performed in order to obtain a diagnosis. This […]
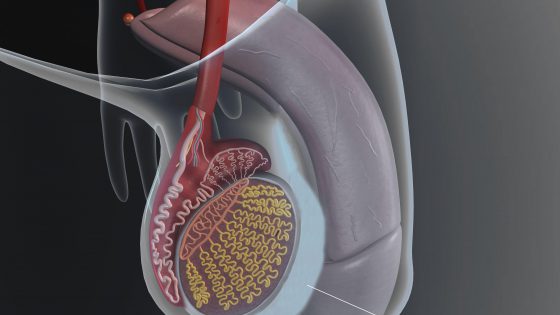
What is a hydrocele? Symptoms and treatment
A hydrocele is the accumulation of fluid in the testicular covers (in one or both testicles) causing an almost permanent swelling of the scrotum. Is not rare in newborns, but they occur more frequently in […]
