Use of platelet rich plasma (PRP) in low ovarian reserve
Low ovarian reserve means a lower probability of spontaneous conceiving, as well as a decrease in the number of eggs obtained in ovarian stimulation treatments. At Instituto Bernabeu, the low ovarian reserve unit works to develop individualized stimulation protocols for this type of patient, together with pharmacogenetic studies (which determine the most appropriate medication according to the genes involved in ovarian response) and technological advances in the laboratory, which make it possible to accumulate eggs in several cycles of stimulation.
However, we know that there’s an endowment of “residual dormant follicles” that cannot be activated with the drugs used during stimulation. Some research suggests that intraovarian administration of platelet-rich plasma (PRP) can activate the ovary (“ovarian rejuvenation“), increasing the number of eggs obtained and reporting cases of spontaneous pregnancies and after in vitro fertilization.
Índice
What is the Platelet Rich Plasma (PRP) and Growth Factors?
It’s a portion of the patient’s own plasma with a high concentration of platelets. It’s obtained after separating the components of a blood sample, in a process known as centrifugation. Platelets release a large number of growth factors, which promote the repair and regeneration of different tissues.
How can you promote ovarian response and “ovarian rejuvenation”?
Development of follicles in very early stages depends on different growth factors, so that the administration of PRP directly in the ovary, would increase their concentration and favour the activation of “sleeping follicles”.

What does the treatment consist of?
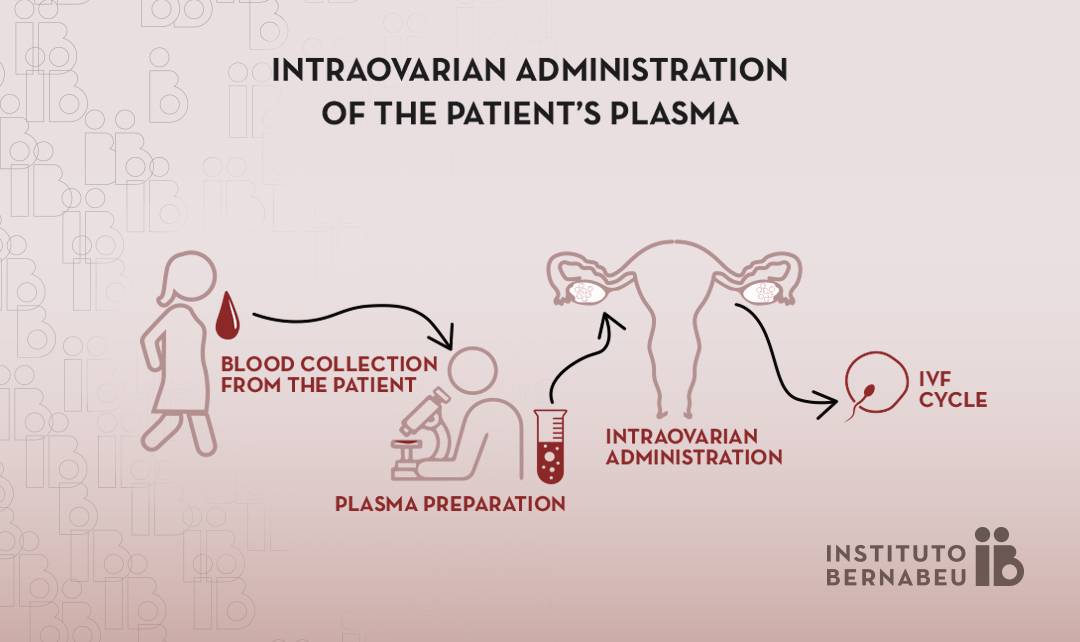
After obtaining a blood sample from the patient, as in a simple analysis, the PRP obtained is introduced into both ovaries by transvaginal puncture under sedation, without requiring hospitalization. It can be administered in the same procedure in which the eggs are extracted, and in patients who are going to undergo subsequent stimulations.
After the procedure, the patients will continue with the prescribed ovarian stimulation treatment, or the corresponding follow-up.
Because the patient’s own blood is used, there is no risk of rejection.
PRP and Growth Factors, ¿Are they indicated for all patients with low ovarian reserve?
It’s an experimental treatment, with promising results, and in which the medical team must assess the appropriateness of its performance in each case, evaluating the chances of success or improvement in the ovarian response. On the other hand, we must bear in mind that no available treatment will improve oocyte quality, mainly depending on age.
Dr Ana Fuentes, gyneacologist at Instituto Bernabeu
THE FOLLOWING MAY ALSO BE OF INTEREST TO YOU:
- Ovarian rejuvenation through fragmentation and transplantation of ovarian cortex
- Poor Ovarian Response Unit
- IBgen IVF. A genetic study of ovarian reserve
- IBgen POF: Ovarian failure genetic Study
- From ovarian rejuvenation to follicle activation, strategies for patients with low ovarian reserve
- Double stimulation: is it possible to recover more oocytes in patients with low ovarian reserve?
- Ovarian stimulation during the luteal phase
- IBgen POF: Ovarian failure genetic Study
