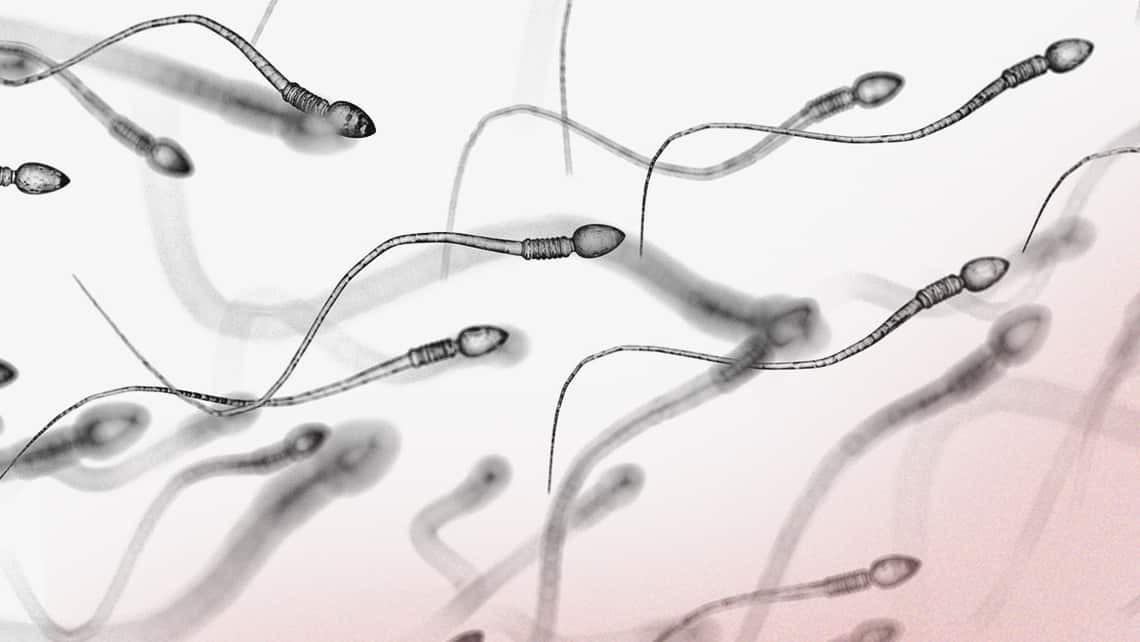
What is the spermatogenesis about?
Spermatogenesis is the process of the sperm formation, which are male gametes. It takes place in the testicular seminiferous tubules with an approximate duration of 62 to 75 days in the human species.
Sperm formation begins around day 24 of embryonic development in the yolk sac, producing about 100 germ cells that migrate to the buds of the genital organs. Around 4,000 of these germ cells accumulate around the fourth week of development, but it will not be until puberty that the testes begin to produce sperm. A process that will continue throughout the life of the man, although the quality and quantity of spermatozoa that are formed through spermatogenesis may decrease over time.
For the production of sperm to be possible, specific hormonal conditions are necessary in which the hypothalamus, pituitary, and testes intervene. The hormones involved in the formation of sperm are testosterone, FSH, LH and Inhibin. So alterations in the secretion of these hormones can result in the sperm not being generated.
The spermatogenesis processes
There are 3 fundamental phases in the formation of sperm:
- Proliferative phase or spermatocytogenesis
- The meiotic phase
- Spermiogenesis phase
In summary, the spermatogenesis process consists of the passage of a germ cell, with 23 pairs of chromosomes (diploid), the spermatogonia, to become a cell with 23 chromosomes (haploid), the spermatozoa. At the end of the whole process, 4 haploid cells (sperm) will be generated from a diploid cell.
The sperm of the testicle, although mature, do not have sufficient capacity to fertilize the oocyte on their own. Rather, they need a series of changes to acquire the capacity for movement and changes at the membrane level to be able to recognize the oocyte. This phase is called training and occurs along the epididymis. Once the sperm are developed and matured, they are expelled in ejaculation. Of which it is estimated that only 25% manage to have sufficient capacity to fertilize the oocyte.
Problems in the spermatogenesis
Now, there are situations in which the sperm formation process in the testicle is altered. Not observing sperm in the ejaculate, which is what is known as secretory azoospermia. The causes can be very diverse:
- Chromosomal alterations: as occurs in Klinefelter syndrome (karyotype 47XXY) or by microdeletions of the Y chromosome, which consists of the loss of genetic material involved in spermatogenesis.
- Bilateral cryptorchidism (incomplete descent of the testes into the scrotal bag)
- Testicular torsions
- Trauma
- Infectious processes (eg mumps in adolescence)
- Radio-chemotherapy treatments
The prognosis in this type of azoospermias is uncertain, and the probability of finding foci of preserved spermatogenesis will depend on many factors.
There are different parameters that have been tried to correlate with the presence of sperm. Such as serum FSH levels, testicular size, or karyotype. Although none of these parameters has been shown to be decisive in the prognosis of the presence of sperm.
In these cases, a careful search for sperm is chosen through a multiple testicular biopsy of both testicles. More conveniently using the MICRO-TESE technique, to increase the possibilities.
IT MAY ALSO BE OF INTEREST TO YOU:
