What is a residual follicle? Diagnosis and treatment of a residual cyst
Residual follicle is the term given to the structure remaining in the ovary following a process of stimulation, whether this has been for insemination or during a cycle of in vitro fertilisation (IVF). Diagnosis is generally carried out using ultrasound imaging.
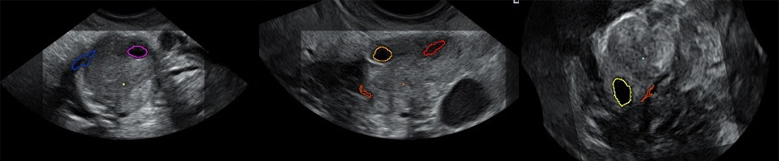
On the whole, before embarking on a course of ovarian stimulation, a basal ultrasound scan is carried out. The aim is to check that the ovary is resting. In other words, that it has antral follicles measuring under 10 millimetres in length.
A resting ovary of this kind with small antral follicles can be observed in the following images.
Once the patient has begun the stimulation cycle for artificial insemination, the aim is to generate between 2 and 3 follicles. However, if the goal is IFV, we will aim to generate a greater quantity of follicles.
Once the procedure has been carried out (whether this be insemination or ovarian puncture followed by transfer), if the attempt has unfortunately been unsuccessful, the patient is once again evaluated during the next menstrual cycle in order to see if a new course of treatment can begin. It is during this evaluation that a residual follicle can appear.
We can find follicles that ought to be small during this stage. However, some are actually already over 10 millimetres in length. If the follicle is between 3 and 5 centimetres long, it is known as a residual cyst. Its aetiology is associated with the absence of ovulation in the follicle during the stimulation cycle or the presence of smaller follicles that continue to grow and remain until the next period.
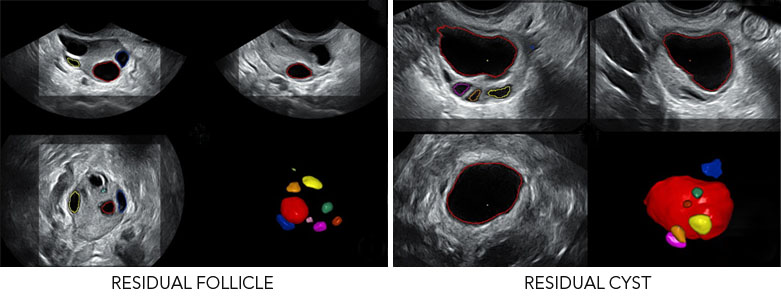
Treatment of residual follicles or cysts of this kind can take a wait-and-see approach consisting simply of waiting for menstruation to take place and checking to see if the structures have disappeared. Or, alternatively, an active approach in which hormonal contraceptives are prescribed in order to block endogenous hormone production and encourage the structure to disappear. Whatever the case, if the structures remain or if the residual follicle or cyst reaches over 5 centimetres in length, specialist gynaecological intervention is required.
Dr Juan Carlos Castillo, gynaecologist at Instituto Bernabeu.
