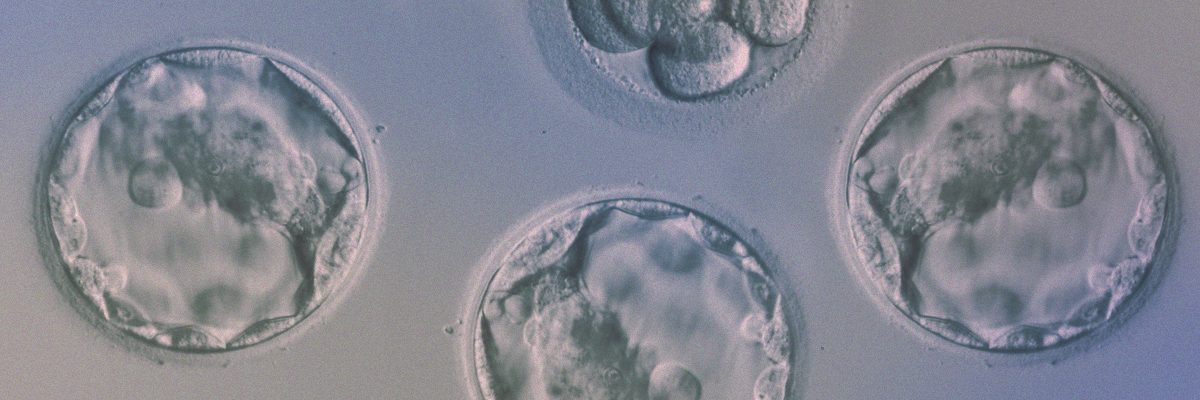
Embryo freezing. Cryotransfer
Embryo freezing by vitrification, allows cryopreservation in optimal conditions in order to have those embryos for future transfers to achieve pregnancy.
Why do we have frozen embryos?
When performing an IVF cycle, our goal is to transfer one or two high-quality embryos to the mother’s uterus. To do this we need to obtain an adequate number of eggs from about 6 to 15 depending on the patient characteristics and her treatment response. We need a relatively high number due to the fact that not all eggs will fertilise and those which do fertilise, not all will develop appropriately in the laboratory during the early stages prior to the transfer. In general the average number of embryos suitable to transfer is close to one third of the eggs originally obtained.
However, the percentage of eggs that fertilise and develop properly is extremely variable and sometimes fertilisation rates are high and the development of embryos in the laboratory is optimal. In these cases several embryos are suitable for transfer on the day of transfer. Nevertheless we can only use one or two embryos for the transfer. The rest of the high-quality embryos are “cryopreserved”, i.e. they are frozen in order to be used in future transfers while retaining much of their potential to achieve pregnancy.
What is the cryopreservation process?
Embryo freezing has been part of the IVF process since the first treatments began but unfortunately the results were very poor on embryo survival and thus pregnancy rates were very low. This was mainly due to the formation of crystals in the interior of the embryo often leading to its structure being damaged and resulting in a very poor prognosis. In recent years cryobiology has made substantial progress as well as the new techniques used to preserve embryos. These techniques are known as “vitrification” and prepare the embryos with high concentrations of protective substances that make the liquid medium prevent the formation of intracellular ice.
At Instituto Bernabeu, each patient has their embryos arranged in a unique location in the cryo tanks, which is not shared with other samples or patients, so that they are safeguarded from possible cross contamination or impairment.
What is embryo vitrification?
Vitrification is an ultra-rapid freezing technique based on the use of very high concentrations of cryoprotector and extremely high rates of cooling, which prevent ice crystals from forming. Its implementation as a routine technique in laboratories has contributed to a spectacular improvement in results, compared to other techniques traditionally used, as well as an increase in survival rates to 90%.

What is the difference between fresh embryo and frozen embryo transfer?
Although the results for frozen embryo transfers are a bit lower than those for fresh embryo transfers, advances in freezing techniques are making the difference less marked. Furthermore, embryo freezing does not correlate with a higher risk of suffering anomalies or complications during pregnancy when compared to the general population.
What is the treatment process involving frozen embryos? How is a “CT” programmed?
Treatment with frozen embryos is simple, convenient and economical. It does not require multiple daily injections or ultrasound scans. There is no need for sedation and there are no side-effects in the vast majority of cases. This is due to the fact that hormone levels during preparation will be very similar to those of a normal cycle.
Treatment is based on the preparation of the uterus of the mother at the time of thawing and transfer of the cryopreserved embryos.
The two most commonly used methods of endometrial preparation are the artificial cycle (with hormonal treatment) and the natural cycle. Both treatments have the same reproductive results and your doctor will recommend which is most appropriate based on your medical history.
Transfer of frozen embryos in an artificial or substituted cycle
The artificial cycle starts with menstruation and is based on the administration of oestrogen orally or transdermally (in the form of patches or gels) for a period of about two weeks before the transfer. Some times, your Doctor may also indicate the administration of a single injection prior to start of treatment. Once an adequate response to the treatment has been verified, vaginal progesterone eggs (sometimes also subcutaneous) will be added and the cryotransfer will take place after uterine exposure to progesterone for the number of days equivalent to the development of the embryo we are going to use. On the day of the cryotransfer or the days prior to it, a blood test will be carried out to check the progesterone levels in the blood. Generally, the medication will be maintained until the 10th-12th week of pregnancy.
Transfer of frozen embryos in natural cycle
Preparation of endometrium in the natural cycle is achieved through the hormones (oestrogen and progesterone) produced by the growing ovarian follicle, which is why regular menstrual cycles are essential for this treatment. It will be necessary to monitor the ovarian cycle by means of one or more ultrasound scans until the follicle that is going to ovulate is detected. Ovulation is triggered by a single injection of HCG. Cryotransfer takes place one week after ovulation. As supportive treatment, low-dose vaginal progesterone eggs are added the days prior to the cryotransfer and maintained during the first trimester. This treatment has the advantage of not requiring any medication.
The embryo transfer technique is identical to that used for fresh embryos and does not require different preparation or additional discomfort. Subsequent recommendations are the same and the individualised treatment should be continued at least until a pregnancy test is performed.

What are the chances of success in achieving pregnancy with frozen embryos?
In recent years with the introduction of vitrification, embryo survival rates and pregnancy rates have improved considerably and have even exceeded the most optimistic viewpoints.
Keep in mind that the chances of achieving pregnancy in IVF vary greatly depending on the type of treatment and the partners’ characteristics (age, cause of infertility, etc.). The success rates are individual to each case. The success rate is slightly lower than that obtained with fresh embryos.
Once pregnant, should I take special care? Will the unborn child be at risk?
The data on pregnancies and children born after frozen embryo treatments shows no difference to those using embryos transferred without prior cryopreservation. Therefore there is no evidence against the performing of this type of treatment.