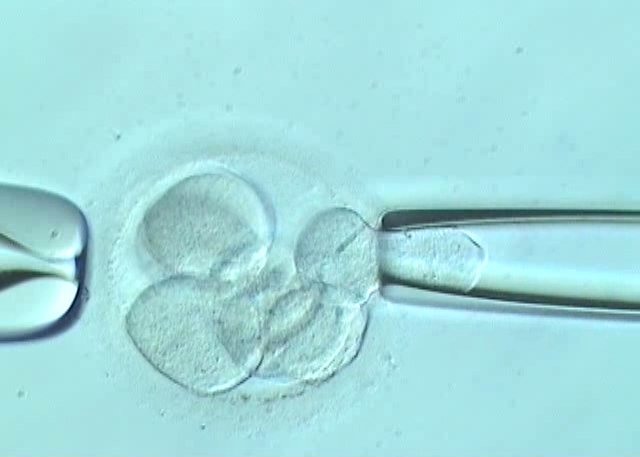
The latest in pre-implantation genetic diagnosis (PGD)
Pre-implantation genetic diagnosis(PGD) consists of studying chromosomalabnormalities and genetic abnormalities in the embryo prior to transfer to the mother. Itspurpose is to ensure that children are healthy and to bring thetransmission of a given condition to an end.
Significant progress that has revolutionised this area ofreproductive medicine has been made over the last few years and specificallywith regards to one type of PGD called PGT-A (pre-implantationgenetic diagnosis for aneuploidy analysis).
Only embryos with the correct number of chromosomes can lead tothe birth of a healthy child. All others end in embryo arrest or pregnancy loss. In the human species, thecorrect number of chromosomes is 46 and 23 of these are inherited from thefather and a further 23 are inherited from the mother. Traditionally, in thefirst version of PGT-A, the most commonly used technique was fluorescence in situ hybridisation(FISH). It only facilitated analysis of some chromosomessimultaneously (X, Y, 13, 15, 16, 17, 18, 21 and 22) and it had a number oftechnical limitations.
Significant progress has been made over the last few years in the field of molecular biology and these have led to the development of techniques that facilitate analysis of all the chromosomes using just one or a few cells. This is the case in embryo biopsies.
The first ground-breaking technique in molecular biology usedfor PGT-A was array CGH (comparative genomichybridisation on isolated DNA samples). This technique can be used to detectincreases or decreases in genetic material. As such, it can be used to identifyany changes in any of the embryo’s chromosomes. Use of this technique in PGT-Awas an important step forward since, on the contrary to FISH, it was possible to studyincreases or decreases in any chromosome.
More recently, development of next generation sequencing techniques (NGS) has made it possible to obtain a large number of sequences from a small quantity of DNA. These can be used to reconstruct the molecular karyotype of the embryo and it is possible to understand if there are increases or losses in any of the chromosomes. The main advantage of NGS techniques applied to PGT-A is their increased resolution. That is, their capacity to detect increases or decreases in DNA of a smaller size.
Furthermore, these recent techniques have made it possible tobetter highlight a phenomenon found in human embryos, specifically chromosomal mosaicism (when the embryo hasa mix of chromosomally normal and abnormal cells). Both array CGH and NGSpermit detection of chromosomal mosaicism. The latter, given its increasedresolution, is able to detect low percentage mosaicism.
Therefore, development and use of new molecular biology techniques such as array CGH and NGS have led to huge progress in PGT-A, making it a diagnostic tool that can detect almost any numerical chromosomal abnormality in couples who are at risk of producing abnormal embryos.
At Instituto Bernabeu, we offer these ground-breaking techniques (array CGH and NGS) applied to PGT-A with the aim of guaranteeing the very best results for our patients.
Dr Belén Lledó, Medical Director of IBBIOTECH, part of the Instituto Bernabeu group.
