Reproductive biology
Discover in depth the biological processes related to fertilization, embryo implantation and all aspects affecting human reproductive biology.
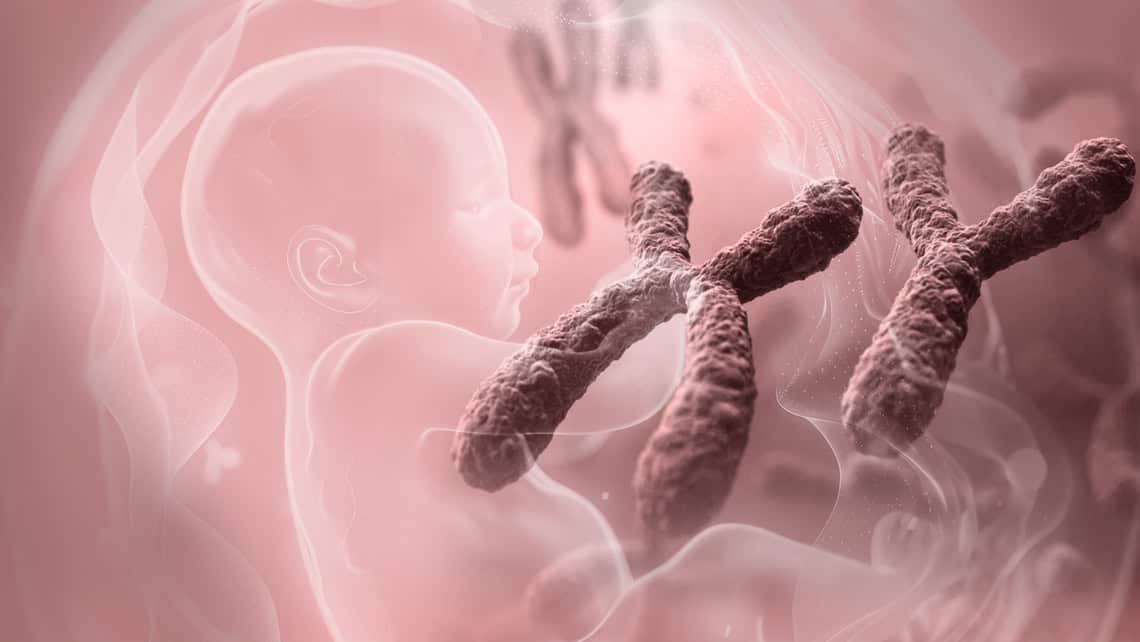
New Genetic Evidence on Pregnancy Loss:
Genetic Variants and Aneuploidyicas: new keys to understanding pregnancy loss Aneuploidy—the presence of an incorrect number of chromosomes in embryos—is the leading cause of pregnancy loss and genetic disorders such as Down syndrome. Although its […]

By not using external gamete banks, we can guarantee that none of our patients have received these semen samples. An unprecedented medical scandal has rocked Europe: a single sperm donor, carrier of a genetic mutation […]
Complementary or add-on treatments in cases of low ovarian reserve
Low response to ovarian stimulation is a medical challenge, as the number of oocytes retrieved is a key factor in the success of in vitro fertilisation.Low ovarian response is considered to be when fewer than […]

World Patient Safety Day: Instituto Bernabeu reaffirms its commitment to excellence in care
Every September 17th, we commemorate World Patient Safety Day, an initiative driven by the WHO. This year, 2025, under the theme “Act Together for Safety,” it invites us to reflect on and strengthen the responsibility […]

The Microbiome and Fertility: A Key Relationship
The microbiome is the collection of microorganisms that live in our bodies and influence important functions like digestion, immunity, and protection against infections. In recent years, it has been discovered that it also plays a […]
Vaginal probiotics: what they do and how they help to achieve pregnancies
The microbial species in a woman’s vaginal flora play an important role in good health and prevention of infections. Over 50 microbial species have been identified. Personal hygiene and a healthy, balanced diet are key […]
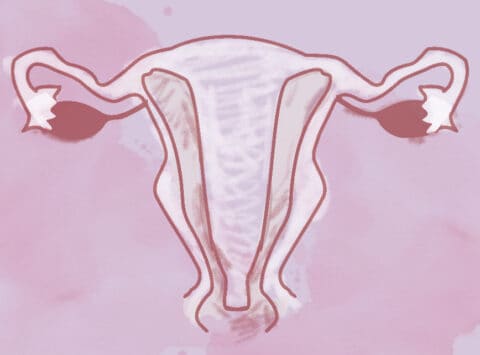
Septate Uterus: what it is, how it is diagnosed, and its treatment
The uterus, fallopian tubes and vagina (or at least part of it) come from embryonic structures called Müllerian ducts. These are two tubular formations which appear on each side of the body, which join at […]
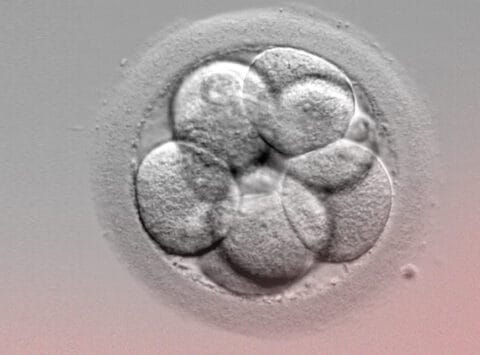
Embryo transfer: How many embryos should be transferred?
In recent years, thanks to long culture and the use of time-lapse incubators, we have been able to preserve embryos in the in vitro fertilisation (IVF) laboratory until day 5-6 of embryo development. This has […]
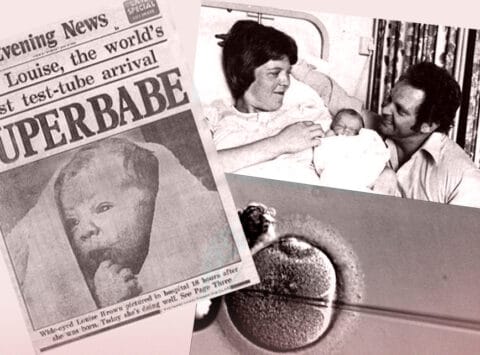
The assisted reproduction in humans that we are familiar with today would not have been possible without the discoveries made over 70 years ago.
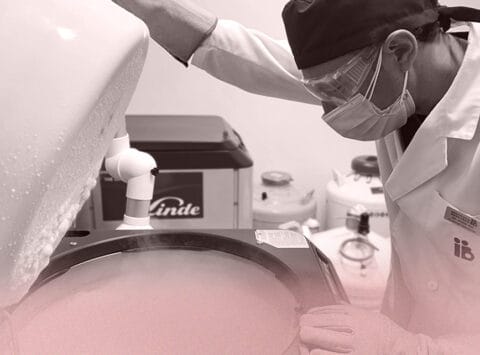
Simulating the conditions in the uterus. IVF laboratory controls
Specific management and quality control systems are key factors in increasing success rates at in vitro fertilisation laboratories (IVF laboratories). Since 2006, all Instituto Bernabeu clinics have adhered to official international ISO 9001 quality management […]
