What happens to ova that have not fertilised?
During assisted reproduction treatment, the ova and spermatozoa need to be transported to a laboratory where they are united using one of two methods: conventional in vitro fertilisation (IVF) or intracytoplasmic sperm injection (ICSI).
During IVF, ova and spermatozoa are brought into close contact so that a spermatozoon can penetrate the ovule ‘naturally’ and generate fertilisation. It is a mainly physiological process but, nevertheless, it does not always work and this is generally due to semen quality or oocyte quality issues. In these cases, we use an alternative technique in order to achieve fertilisation.
ICSI consists of inserting a previously-selected spermatozoon into a mature ovum using a micropipette. When gametes are not optimum quality, this tends to be the preferred method.
Índice
Fecundation process reactions
However, the aforementioned processes do not guarantee fertilisation in all cases. In fact, according to quality indicators established by the Spanish Association of Reproduction Biology (ASEBIR),
- minimum fertilisation in a woman’s own oocyte is 58.1%,
- desired fertilisation is 63.2%
- and optimum fertilisation is 73.5%.
In the case of donated oocytes, these percentages can reach
- up to 66.3% minimum fertilisation,
- 70.3% desired fertilisation
- and 78.9% optimum fertilisation.
However, between 1 and 3% of cases result in absolute fertilisation failure when no fertilised ova are obtained.
In order to determine if fertilisation has taken place or not, we need to wait between 16 and 18 hours following either of the aforementioned techniques. Outside the boundaries of this period, it is impossible to know if the oocyte has fertilised or not and, in fact, there is a risk of incorrectly assessing the situation.
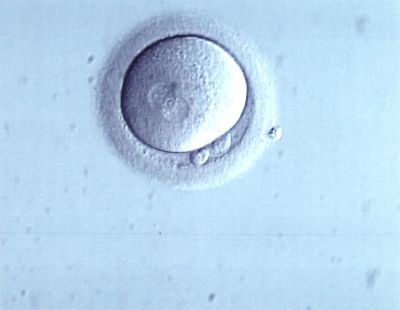
Oocyte’s normal fecundation
When fertilisation takes place under normal circumstances, there are two structures inside the ovum known as pronuclei. One comes from the mother and the other comes from the father.
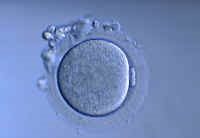
Abnormal fecundation
However, abnormal fertilisation is also common. This is the case when, instead of two pronuclei, there is one, three or even more. Abnormalities such as these are an indication of possible abnormalities in the future embryo’s genetic material and this is why these ova are rejected once fertilisation has been assessed.
Images from left to right: Fertilised ova (2 pronuclei), abnormal fertilised ova (3 pronuclei) and non-fertilised ova.
No oocyte’s fecundation
Last of all, there can be non-fertilised ova that do not have any pronuclei. A number of changes need to take place inside an ovum in order for it to fertilise. Therefore, if the spermatozoa is unable to activate those changes or the ovum is unable to generate them, then fertilisation does not take place.
Over the last few years, in vitro oocyte activation techniques have been achieved through the use of a calcium ionophore culture medium. This encourages the activation process to start and it can help to achieve improved fertilisation rates. However, it is still currently an experimental technique and additional studies are needed in order to confirm that it is safe.
Unfolding progress and development of new reproductive medicine techniques are a source of hope for couples who wish to pregnant and give birth to a healthy child.
THE FOLLOWING MAY ALSO BE OF INTEREST TO YOU
- In Vitro Fertilization (IVF)
- Poor Ovarian Response Unit
- Double stimulation: is it possible to recover more oocytes in patients with low ovarian reserve?
- Accumulation of oocytes in patients with a low response.
Nerea Díaz, a biologist at Instituto Bernabeu