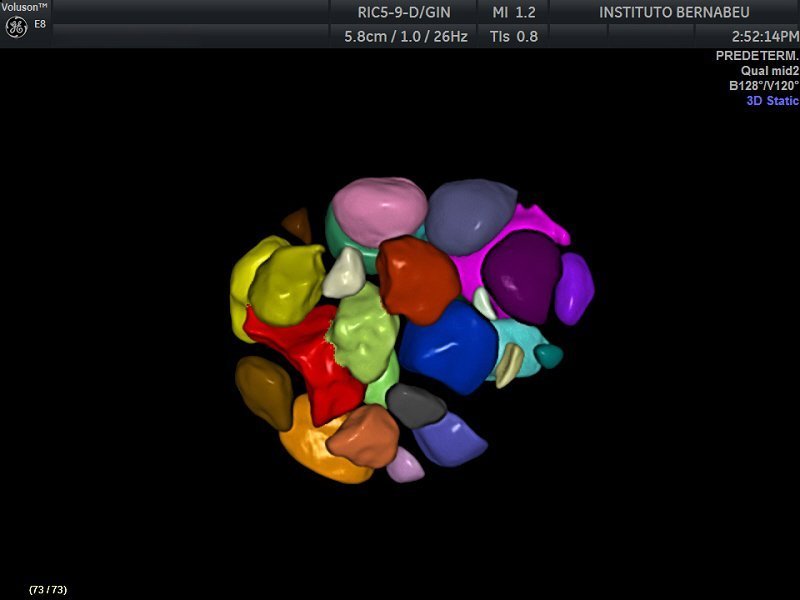
Ovarian Hyperstimulation Syndrome
Ovarian hyperstimulation syndrome is a complication of ovarian stimulation needed for in vitro fertilization. This complication can become very severe but is also very rare, being reduced lately to less than 1% since effective strategies to avoid it has been achieved and implemented.
Índice
Cause of ovarian hyperstimulation syndrome
Prior to start of the symptoms, the hormones used in the treatment cause the fluid to accumulate around the ovaries. This happens usually in ovaries that reach a high number of stimulated follicles, although it is not a required state for its initiation.
Then, as a consequence of the last medication administered prior to the collection of oocytes (recombinant hCG), the levels of oestradiol are perpetuated and the mechanisms that cause the hyperstimulation syndrome are triggered.
However, the condition only appears in less than 5% when there is no pregnancy, being 95% of the cases after the administration of recombinant hCG and subsequent embryo transfer with pregnancy result.
Risk factors
Eventually, factors that determine a higher risk of the syndrome have been identified. They are, for example:
- A high number of stimulated follicles
- Suffering from Polycystic Ovary Syndrome
- Having a low body mass index or
- Reaching high levels of estrogen after completing treatment
Symptoms of Hyperstimulation Syndrome
Although, as previously mentioned, it can cause an extremely serious condition compromising the health of the patient, it more frequently appears in mild or moderate form. The most frequent symptoms are:
- The abdominal distention
- Nausea with or without vomiting
- Diarrhea
- Choking feeling
- The perception of urinating less with weight gain
The symptoms in their most severe version have been noted as:
- Extensive generalized thrombosis
- Massive pleural effusion (fluid in the lung)
- Ascites (fluid in the peritoneal cavity)
- Kidney failure and even death
Treatment of Ovarian Hyperstimulation Syndrome
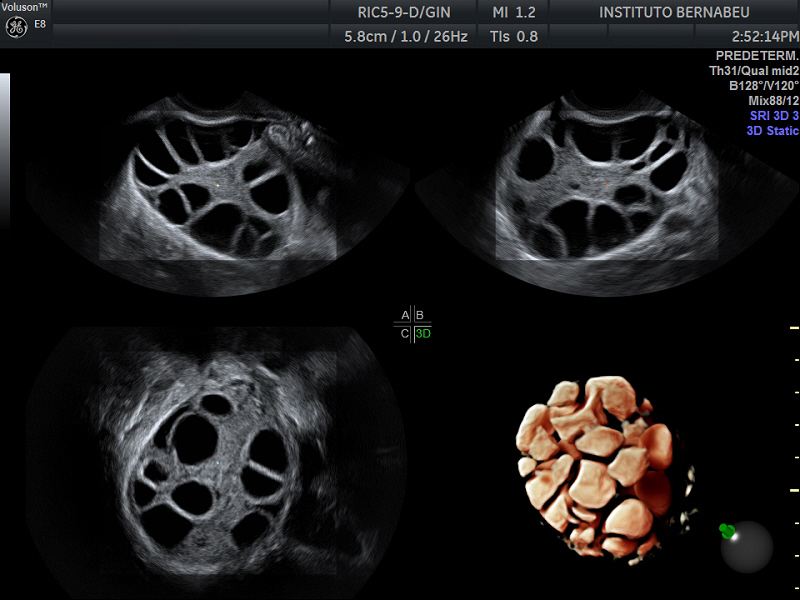
Certainly, the biggest fear is related to the fact that there is no effective treatment. Therapy consists of controlling the symptoms that appear: anticoagulants to prevent thrombosis, emptying lungs and peritoneal cavity of fluid when they are full, administrating diuretics in the event of renal failure… and even, in some extreme cases, terminating the pregnancy has been considered a definitive therapeutic strategy.
Strategies that currently prevent Ovarian Hyperstimulation Syndrome
Strategies are now so effective that this complication, which has caused so much concern in the reproductive medicine sector, has been practically eliminated.
- First and foremost, the use of GnRH agonist, instead of recombinant hCG to trigger ovulation in order to effectively collect oocytes. The GnRH agonist makes the hormones last less time, so without other treatment it usually causes menstruation after 6-7 days after its administration.
- Second, the vitrification of embryos. In a state when the patient is likely to suffer from Ovarian Hyperstimulation Syndrome, a gestation could trigger the appearance of serious complications. Occasionally, cases of this condition have been reported in spontaneous pregnancies, without having received any treatment.
MAY ALSO BE OF INTEREST:
- What are the potential complications associated with IVF?
- Does ovarian stimulation for in vitro fertilisation treatment increase the risk of gynaecological cancer?
- What can we see in ultrasound scans: follicles or oocytes?
Dr. Belén Moliner, gynaecologist of Instituto Bernabeu
