Blastocyst embryo: What it is, advantages, types and classification according to its quality
Índice
What is a blastocyst
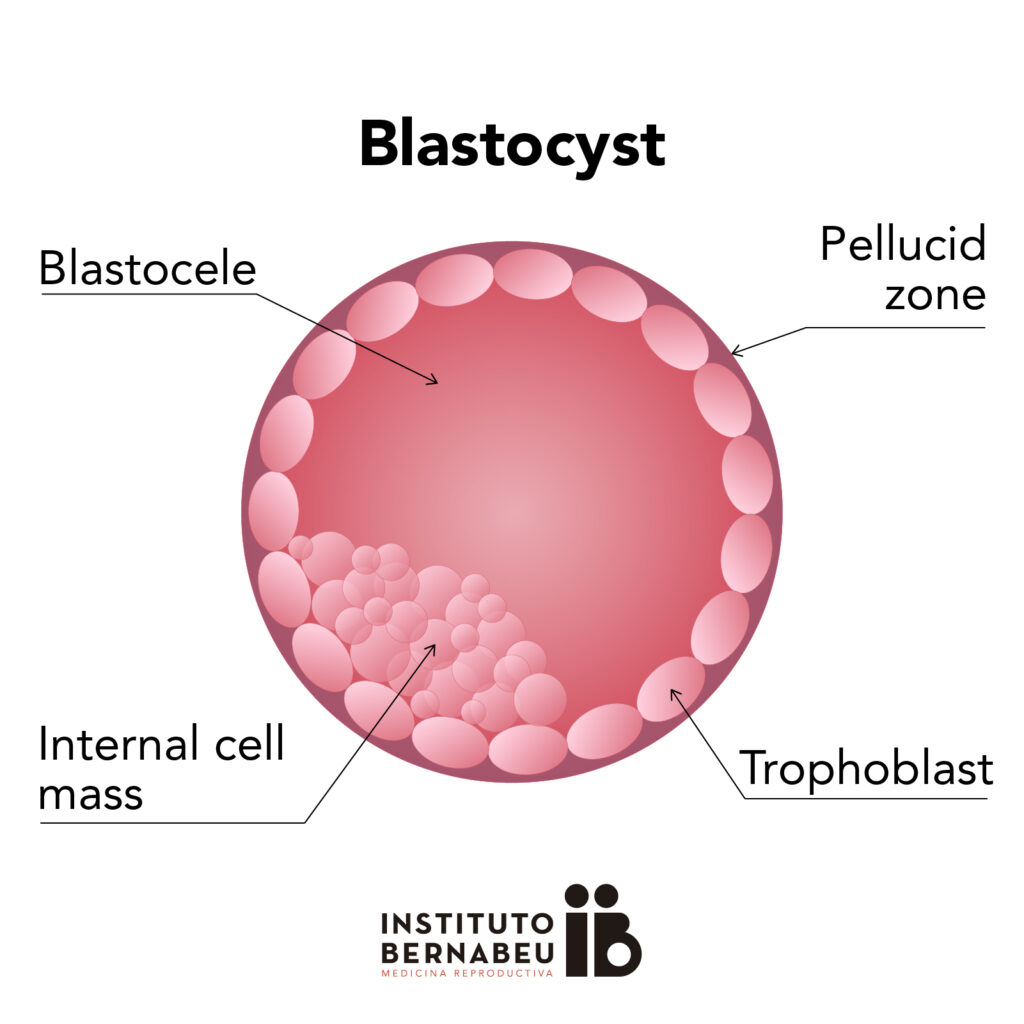
A blastocyst is a 5/6 day embryo with a complex cell structure consisting of approximately 200 cells. The blastocyst stage is the stage of development prior to the implantation of the embryo in the mother’s womb.
This cellular structure differs in two areas that will clearly determine the quality of the embryo and its options to implant and achieve a pregnancy:
– The first is the internal cell mass (ICM), which is a group of cells found inside the blastocyst or cavity that will give rise to the fetus.
– The second is an epithelial cell layer that covers the blastocele, called the trophoectoderm (TE), which will give rise to the extra-embryonic tissues (placenta and amniotic membranes).
Several cells of the TE are usually biopsied when we perform a Preimplantation Genetic Test (PGT-A) and are analyzed by Next generation sequencing (NGS) to make a selection of those embryos free of chromosomal alterations. As we will see later, to assess and classify the quality of a blastocyst we base on its size or expansion of the cavity or blastocele and on the morphology of the ICM and TE.
Advantages of transferring a blastocyst embryo: Natural selection of the best developing embryos
Transferring a blastocyst has the following benefits:
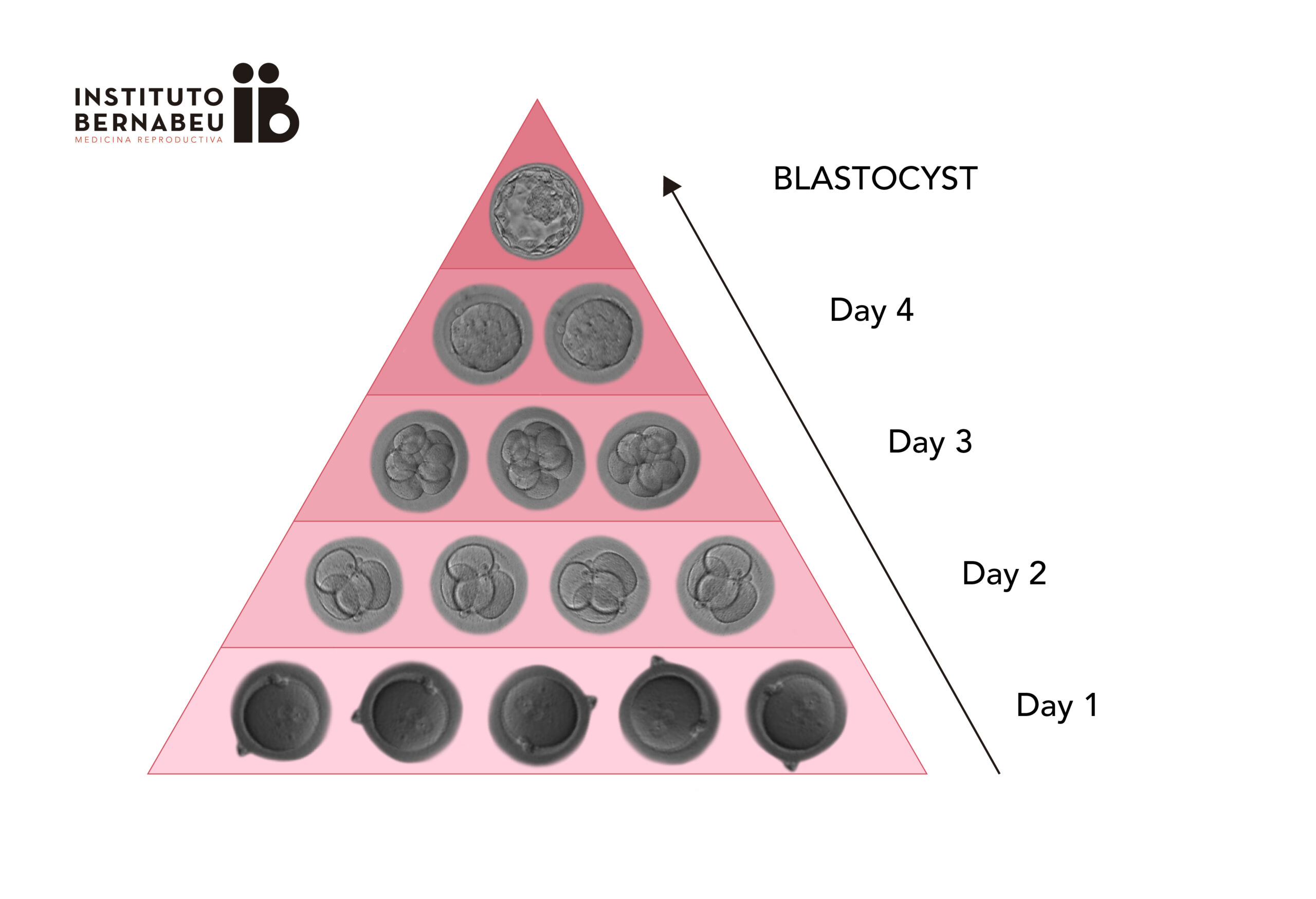
- A better embryo selection is possible. The embryos that reach this stage have a greater capacity to implant and achieve an evolutive pregnancy, since they have overcome possible developmental blocks that usually occur in the early stages.
- That is why we usually limit the number of blastocysts in each transfer to 1, avoiding the risk of a multiple pregnancy.
- The development of new media and better culture conditions allow us to reach blastocyst formation percentages above 60%. The optimization of vitrification techniques guarantees the freezing in the blastocyst stage with high success rates.
- There is a better physiological synchronization between the embryo and the endometrium, since it is naturally at this stage that the embryo reaches the uterine cavity. In addition, there is a lower percentage of uterine contractions at the time of transfer, which favors embryo implantation.
- Due to the selection process mentioned in the first point, blastocysts present a lower percentage of chromosomal alterations or aneuploidies.
- The performance of an embryonic biopsy in PGT-A cycles should be done at the blastocyst stage, since it has been demonstrate that the embryo is not damaged.
Types of classification of blastocysts
The Spanish Association for the Study of Reproduction Biology (ASEBIR) classifies blastocysts into 4 different categories (A, B, C and D) based on the characteristics of the ICM and TE and their expansion. It is also a dynamic classification system that takes embryo evolution into account on day four and/or five of development.
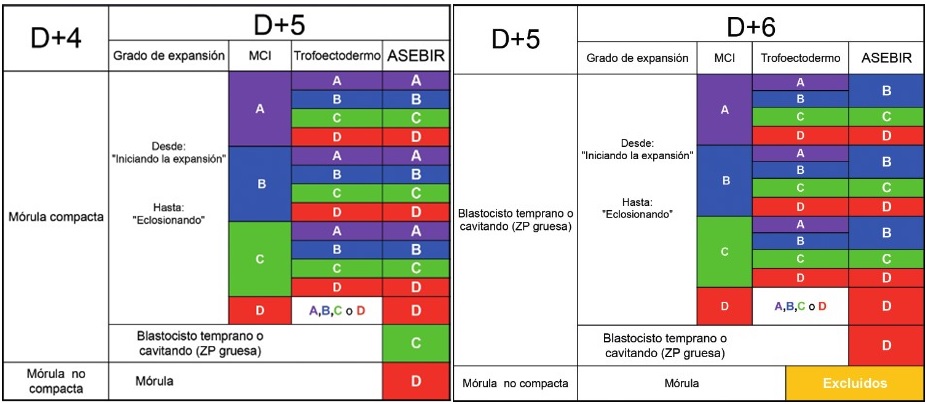
(ASEBIR classification)
Blastocysts that are assigned a category A classification are optimum quality blastocysts that have the greatest ability to implant. Category B blastocysts are good quality blastocysts with an elevated ability to implant. Category C refers to blastocysts with an average quality level and average ability to implant whilst category D blastocysts are poor quality blastocysts that are unlikely to lead to gestation.
However, the most standardised international classification system and the one that is used worldwide is the Gardner and Schoolcraft (1999) classification system. It only takes into account a single observation on the fifth or sixth day of development. Expansion is assessed in 6 stages, from the least to the most. From grade 3 onwards, there is a morphological criteria to divide ICM and TE into 3 categories, from the poorest to the best quality based on the number of cells, their cohesion and their appearance (A, B and C). The best gestation rates are obtained by transferring blastocysts that are quality 4AA or higher.
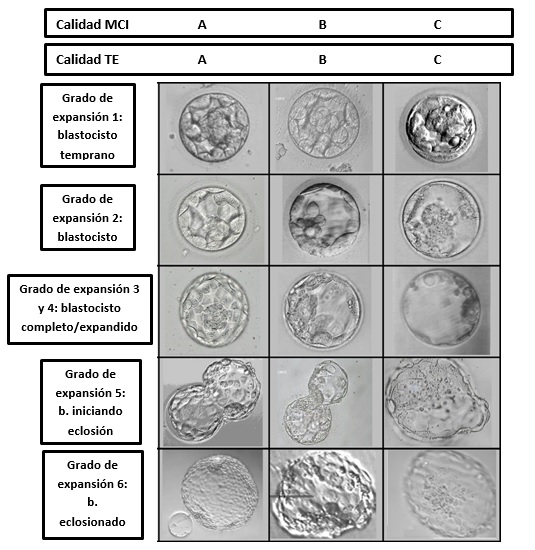
(Gardner and Schoolcraft Classification, 1999)
Apart from a comparison of the blastocyst’s morphology, other morphological criteria for choosing one blastocyst over another can be taken into account. These include the thickness of the external layer (zona pellucida), the presence of signs of eclosion and embryo quality during previous stages.
Embryologist training is key to classifying blastocysts correctly and always transferring the embryo with the greatest ability to lead to gestation.
IT MAY ALSO BE OF INTEREST TO YOU
- In vitro fertilization at Instituto Bernabeu
- Embryo transfer
- Criteria for embryo classification
- Embryonic arrest, why don’t all of my embryos develop equally?
- Embryo normal and abnormal division
- NEGATIVE IVF: Everything you need to know after a failed IVF
Dr Jorge Ten, Director of the Reproduction Biology Unit at Instituto Bernabeu
