
The impact of Turner syndrome on women
Turner syndrome is a chromosomal condition caused by partial or total loss of one of the X chromosomes.
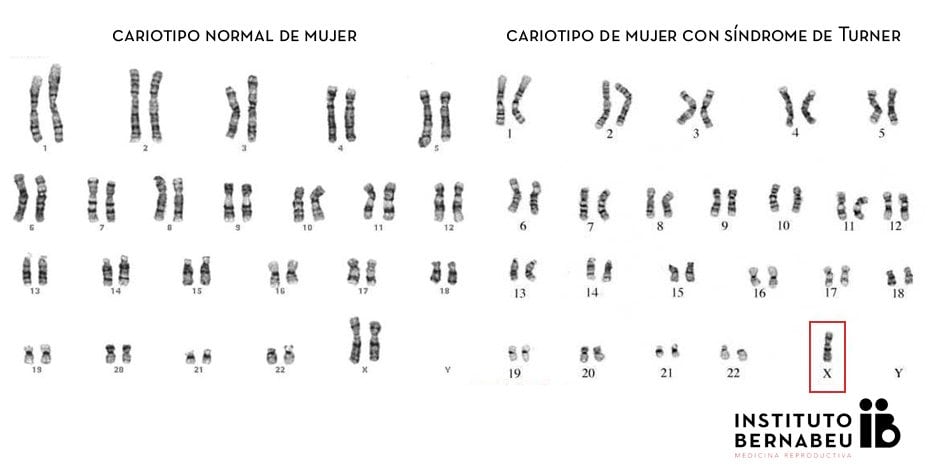
All human beings have 23 pairs of chromosomes and this is what is known as the karyotype. It is where all genetic information is stored. In other words, it is what determines our external appearance, our personal physical characteristics, how our organs work, whether or not we will have certain illnesses and so on. There are 22 pairs of numerical chromosomes ranging from 1 to 22 and one pair of sex chromosomes: X and Y. Women have two X chromosomes – one from their father and one from their mother. Men have one X chromosome – from their mother – and one Y chromosome – from their father. If, when a female embryo is generated, incorrect division leading to total or partial loss of the X chromosome takes place, this generates an abnormal karyotype that is characteristic of women with Turner syndrome. The syndrome, by definition, does not occur in males because they only have one X chromosome and cannot live unless this chromosome is present.
As with all syndromes, Turner syndrome can present itself in a large variety of ways in terms of the affected person’s health but it is generally associated with short stature (< 150 cm) and gonadal dysgenesis (under-developed ovaries). The latter leads to a total or almost total absence of the progenitor cells for ova, causing premature ovarian failure.
In order to confirm a suspected case based on physical characteristics that suggest a woman has the syndrome, a blood sample is taken in order to determine her karyotype. This is the piece of data that can confirm the diagnosis. The ‘standard’ karyotype when one entire X chromosome is absent is 45X0 but there are multiple variants when there is only partial loss of genetic material (mosaic Turner).
Prevalence is estimated to be 1 in every 1,000 embryos (most end in pregnancy loss) and 1 in every 2,500 newborn girls.
As mentioned above, the clinical manifestations can be many and varied depending on the quantity of absent genetic material. The condition’s main features are musculoskeletal (short stature in all cases), swelling in hands and feet, heart abnormalities (in the aortic valve and the exit from the aorta), renal issues, endocrine issues (particularly those affecting the thyroid) and loss of ovarian function in 96% of all cases.
This loss of ovarian function is associated, in the long term, with fertility issues.
First of all, 80 to 85% of affected girls do not experience spontaneous puberty and require hormone treatment with oestrogen. This treatment is also necessary for 15 to 20% of all other affected girls.
It is estimated that between 2 and 7% of affected women will manage to get pregnant naturally but pregnancy loss and malformations in the foetus are more prevalent than in the rest of the general population. This is why providing these women with genetic guidance prior to getting pregnant is recommended.
In most cases, it will be necessary to turn to assisted reproduction techniques in order to achieve a successful pregnancy. The available options include:
- Oocyte preservation (only if the patient has some ovarian function)
- Pre-implantation genetic diagnosis (when the patient is attempting to get pregnant using her own ova)
- Oocyte donation (the most commonly-used technique)
Medical advice indicates that embryo transfer should be performed with just one embryo due to the increased risk of endocrine (gestational diabetes, hyperthyroidism) and heart complications during pregnancy. These complications would be even more serious in a multiple pregnancy. Therefore, before performing treatment, cardiac function and endocrine issues need to be assessed by the corresponding specialists. They must confirm that there are no reasons to advise against pregnancy and, once the patient is pregnant, perform an extensive control of the pregnancy.
Preconception counselling using the aforementioned assisted reproduction techniques and interdisciplinary pregnancy monitoring are essential in achieving maternity for the patient in these cases.
Lydia Luque, a gynaecologist at Instituto Bernabeu.
