Antenatal Diagnosis
Antenatal diagnosis is the number of available methods and techniques to control the development of the foetus before birth.
What is prenatal diagnosis?
The term “prenatal diagnosis” comprises all those diagnostic actions meant to discover a “congenital defect” during pregnancy. Congenital defects are understood as “any abnormality in morphological, structural, functional or molecular development that is present at birth” (although it can also be found later), either external or internal, family-related or random, hereditary or not, single or multiple”.
Types of congenital defects
Around 3% of infants born alive suffer from some type of abnormality. Yet, this figure rises to 4-7% a year after birth. According to the underlying causes, three main types of congenital defects can be identified:
– Chromosomal abnormalities
They are responsible for 12% of all defects. Among them, the most common is Down’s syndrome, which can affect 1 out of every 700 newborns, its frequency being very variable according to mother’s age.
– Hereditary diseases
They make up for 28% of congenital defects. It is already possible for many of them to be diagnosed, using more sophisticated techniques, such as DNA testing. The most frequent techniques in our environment are: cystic fibrosis, myotonic dystrophy, polycystic kidney disease and neurofibromatosis.
– Malformations
They make up for 60% of all congenital defects. They are diagnosed in almost all cases by means of high resolution ultrasound scanning.

What techniques are there for prenatal diagnosis?
So-called “populations at risk” for a given congenital defect are selected by means of “non-invasive techniques for prenatal diagnosis”. Among them, clinical histories, laboratory tests, ultrasound scans and a number of combined tests are found.
If a piece of information or a risk factor is eventually found through the use of non-invasive techniques, confirmation is subsequently sought by means of so-called “invasive techniques for prenatal diagnosis”, thus termed because of the slight risk of foetal loss involved. For this reason, their use cannot be generalised.
Non-invasive techniques for prenatal diagnosis
– Clinic: After writing the patients clinical history, a number of situations may arise in which invasive tests may need to be carried out: advanced age, records of abnormal pregnancies or brain damage, parents with chromosome anomalies, family records of malformations, etc.
– Fetus DNA test in the mother’s blood. The test can be performed from week 10, with the ability to know in two weeks the risk of having Trisomy of the chromosome21(Down Syndrome), Trisomy of the chromosome 18(Edwards Syndrome) and Trisomy of the chromosome 13 (Patau Syndrome) and anomalies related tochromosomes X and Y, such as Turner Syndrome and Klinefelter Syndrome. With a simple blood sample from the mother, some fetal DNA is obtained and can be identified and quantified through an advanced technological process: a massive parallel sequence. Finally, a statistical analysis of having any of the anomalies mentioned is obtained. The sensitivity or reliability of the test is very high, as it has screening rates higher than 99% with false positives lower than 0.1%. It is useful in multiple pregnancies and can be applied to pregnancies achieved after assisted reproduction treatments, including egg donation.
– Blood test. Between weeks 9 and 12 pregnancy proteins can be accounted for. Beta-HGC and PAPP-A (plasmatic protein A), are proteins that must be kept controlled given that any increase or lack of them may be related to chromosome illnesses.
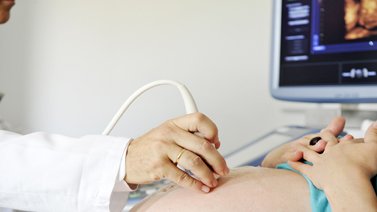
Ultrasound. This method is a very important one for the exploration of antenatal diagnosis and has to be done at specific times during pregnancy:
– First trimester. It allows us to capture images considered “chromosomal abnormality markers”. The most reliable and accepted one is known as “nuchal translucency”, this structure can be visualized at the skin fold behind the nape of the neck between weeks 11 and 14. If it exceeds certain dimensions, (3mm), we will offer you an invasive test. Equally important is to measure the nasal bone since lacking it could be related to Down’s syndrome.
Second trimester. Especially around week 20, time when most anatomic abnormalities can be detected. This must be performed by highly trained professionals. Equipment is also a very important factor as it allows us to detect, through the latest technology: colour Doppler ultrasound and 3-D & 4-D ultrasound, very precise details of foetal anatomy.
– Combined studies. This is called the combined test of the first trimester or EBA-Screening (ultrasound and aneuploide biochemical screening). It consists of a computerized study that calculates the level of risk of any chromosomal abnormality (especially Down’s syndrome), using the age of the pregnant woman, blood test markers (mentioned above) and the measurement of the nuchal translucency. The results show a rate of detection very close to 90%, with an acceptable rate of false positive results of a 3%.
Invasive techniques for prenatal diagnosis
Invasive techniques enable complete diagnosis of many foetal pathologies, especially of chromosomal diseases. They are not exempt from complications, and they involve a certain risk of interfering with the evolution of the pregnancy. Consequently, it is essential to select those pregnancies that can benefit from them. The most commonly used techniques are:
– Chorion biopsy. Its goal is to collect a sample of placenta tissue, either abdominally or transcervically, in order to test foetal chromosomes or to perform more sophisticated tests on DNA or foetal enzymes, for example. It has a clear advantage compared to amniocentesis: it is performed earlier, between weeks 11 and 12, while their complication rates are similar.
Advances in the field of Molecular Biology have made it possible to test those chromosomes that are most frequently involved in numerical alterations in newborns by means of a technique known as Fluorescence In Situ Hybridization (FISH), which is completed within 24-48 hours using the same collection technique. The chromosomes involved are #13, #18, #21, X and Y. In this way, In Situ Hybridization can help us to rule out more than 90% of chromosomal pathologies in a very short time frame.
– Amniocentesis. It involves collecting the amniotic fluid that surrounds the foetus by means of a puncture through the mother’s abdominal wall. It is performed between weeks 15 and 18. The fast method mentioned above (FISH) can also be used, or, alternatively, the definitive long-term culture of all the chromosomes, whose results take two or three weeks.
In both techniques mentioned (Chorion biopsy and Amniocentesis) and in some cases, a longer, more thorough study can be completed by using the most innovative molecular technique, which we also incorporate at Instituto Bernabéu: Array-CGH. It is the safest, most effective way to analyse an individual’s whole genome, in search of gain and loss alterations of DNA. It is being used not only in prenatal diagnosis and pre-implantation diagnosis, but also in the field of Clinical Genetics: cancer, intellectual disability and congenital polymalformative syndromes.
– Cordocentesis. It involves collecting a sample of foetal blood by means of puncture of an umbilical vessel, with ultrasound guidance. It is performed after weeks 19 and 20. A technique that is indicated much more selectively, it is useful for fast testing of foetal chromosomes and confirmation of infections or severe diseases in the foetus.
It is especially useful in pregnancies where there is a risk of foetal hematologic disorder (anaemias, thrombopenias), in which case foetal blood becomes a unique source of information. The only disadvantage is that it normally has a high failure rate of blood collection, as well as a foetal loss rate of around 2% or even higher.